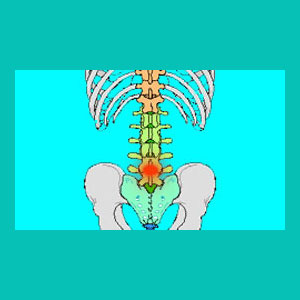
A herniated disc L4-L5 is one of the most common lower back pain diagnoses in existence. L4/L5 is an area of universal degeneration and is the second most prevalent location for a herniation to occur in the human spinal column. When nerve root impingement occurs at this level, sciatica is one of the possible results, regardless of whether the nerve tissue is compressed in the foraminal space or within the central canal itself.
However, the truth is that most lumbar disc herniations are not the actual underlying source of any pain and even when they are, that pain should resolve rather quickly and completely, not cause the ongoing suffering so commonly reported by patients.
This discussion will profile disc prolapse at L4/L5 and provide a comprehensive clinical picture of this highly usual disc abnormality.
Herniated Disc L4-L5 Definition
The L4/L5 intervertebral level separates the L4 vertebra from the L5 spinal bone. Typically this is the last disc fully present in the normal lumbar spine, prior to the lumbosacral junction, which is marked by the L5/S1 disc, also known as the lumbosacral disc. L4/L5 endures considerable disc deterioration as a normal part of its lifespan and degenerative disc disease at this level is normal, generally asymptomatic and virtually universal.
In a herniated L4/L5, the disc has bulged or ruptured and is most commonly blamed for enacting symptoms through the process of foraminal stenosis, which is also called a pinched nerve. However, it is also possible that a herniated disc at this level can be blamed for causing spinal stenosis pain by impinging on the multiple nerves composing the cauda equina, since the actual spinal cord does not exist in the low lumbar region.
Disc Prolapse L4-L5 Causation
The L4/L5 level is the second most common scapegoat disc, only being beaten by L5/S1. So many disc abnormalities can affect L4/L5, but most are nothing of note.
Lumbar degenerative disc disease is a condition which affects every normal human, usually by the age of 30 and often far younger. I was diagnosed at the age of 16. DDD in the lumbar spine, combined with the significant forces which are endured by these discs as we move throughout our lives, set the perfect circumstances for herniated discs to occur. These herniations are typically not problematic, but can be troublesome in some cases. However, it is truly rare that even the most painful herniations create chronic disc pain concerns, although they often take the blame for them.
It is crucial to always keep in mind that herniations can only enact symptoms when they influence a nearly nerve structure. If this does not occur, then the disc bulge is unlikely to create any problems at all.
Herniated Disc L4-L5 Guidance
I get letters from readers every day with MRI results indicating a herniated disc at L4/L5. Typically, these herniations are either diagnosed as causing a mild narrowing of the neuroforaminal space or impinging on the thecal sac. Neither of these conditions is unusual or inherently painful, so to blame severe and chronic back pain on the poor maligned disc is a medical travesty and nothing short of iatrogenic error.
If this represents your diagnosis and a plethora of attempted treatments have not provided you with lasting relief, then I urge you to consider the obvious: The disc may be herniated, but that is not unusual and it is certainly not likely to be the actual explanation for your pain.
L4/L5 and L5/S1 were the first 2 diagnosed herniations in my own case, dating back over 25 years. Although many doctors had told me that I was a surgical emergency case and faced imminent disability, none of these dire predictions came to pass. Now, with a total of 12 herniations in my spine, I am so happy I never acquiesced to these scare tactics and risked my health and very life just to put some extra money in these doctors’ pockets via surgical butchery.
Herniated Disc > Herniated Disc Injury > Herniated Disc L4-L5





