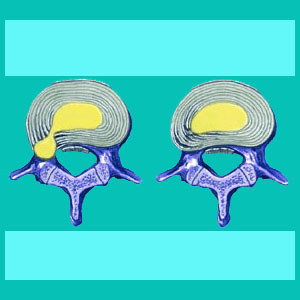
A paramedial herniated disc is also known by several other names including posterolateral herniated disc, paramedial disc bulge, paramedian bulging disc and paramedial disc protrusion. This condition, regardless of the exact diagnostic terminology used, is the most common type of herniated disc in existence, particularly in the lumbar and cervical spinal regions.
While it is not crucial to fully understand the nature of a posterolateral herniation when compared to a far lateral or central disc herniation, it is always a good idea to learn the basics about disc bulges in order to better your chances for successful resolution of your pain. After all, each type of herniation can produce different effects on different types of nerve tissue.
This essay examines the specific paramedian variety of bulging disc in the spinal column.
What is a Paramedial Herniated Disc?
Paramedian disc bulges describe herniations which are off center and asymmetrical in their bulge pattern. These herniations can affect the right side or left side of the disc and generally enter into the lateral recess on the side of the spinal cord.
In some cases, paramedian herniations are said to impinge upon the thecal sac, typically on the frontal/side surface. In rarer cases, these herniations may actually impinge upon the spinal cord itself. Other common speculative or verified diagnostic terms used in conjunction with posterolateral herniations include crowding, impinging or compression of a nerve root, typically in the lateral recess, although sometimes in the neuroforaminal recess.
Remember that herniations which fully or partially block the foraminal space are often referred to as foraminal herniated discs.
Paramedian Bulging Disc Classification
Paramedial disc bulges may be broad based or focal in nature. The vast majority are not problematic or pain-inducing in any way and of those which are symptomatic, many will not require any special care, but will likely improve with time alone.
Some herniations may require professional medical treatment and a few may even be indicated for herniated disc surgery intervention. This is particularly true for severe and verified instances of pinched nerves or spinal stenosis enacted by a bulge which actually compresses the spinal cord itself.
Remember to compare any actual symptoms with the clinical expectations of the diagnosis in order to improve the chances for successful treatment, no matter which path to therapy path you choose to traverse. If the symptoms do not correlate to the diagnosis, then any treatment is unlikely to prove successful.
Paramedial Herniated Disc Experiences
I am happy to see you all increasing your specific knowledge of herniations by reading pages such as this one. Most of you probably ended up here when searching for terms on your MRI report, which is always advised.
You need to understand your diagnosis in order to become active in your own care and you need to become active in your own care in order to recover from a herniated disc. Just remember that no particular type of herniation is inherently any worse than any other and most are still non-issues in terms of causative potential for chronic back pain.
If you have been actively pursuing disc pain care for months or years without relief, there is a good chance that the bulge is not the problem after all. Never forget that misdiagnosed herniated discs may surely be present, but are not the actual source of pain in a great number of patients.
Herniated Disc > What is a Herniated Disc > Paramedial Herniated Disc




