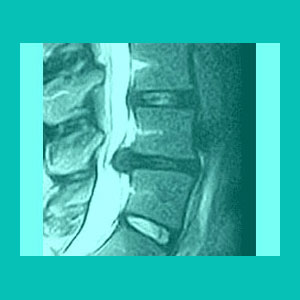
A ruptured disc occurs when the outer wall of the disc, called the annulus fibrosus, tears or breaks, allowing some or all of the soft inner core, called the nucleus pulposus, to leak out of the disc structure. Intervertebral rupture might occur spontaneously due to tremendous traumatic force or might be the end result of normal degenerative changes occurring in the disc. Statistically, disc ruptures are no more problematic than contained bulges. In fact, in some rare cases, when a disc ruptures, it may actually relieve symptoms brought about by structural nerve compression.
This essay examines the occurrence of spinal disc rupture and the effects it might produce in the anatomy of the vertebral column.
Ruptured Disc Condition
Most disc ruptures occur in spinal discs which are already herniated. Any disc bulge creates a weakness in the annulus fibrosus, compromising its structural integrity. This weakness can be exploited by progressive degeneration over time or with significant trauma to the affected area.
If too much pressure builds up on the compromised annulus fibrosus, it is likely to develop an annular tear. This is basically a rip or hole in the outer layers of disc. Remember that this tough outer disc wall contains the nucleus pulposus and once compromised, the nucleus can be squeezed out of the disc akin to toothpaste.
Alternately, the normal processes of disc degeneration include the drying out of the disc structure. These changes can make the disc increasingly brittle and more prone to developing cracks in the annulus fibrosus. In turn, these cracks can also create a disc rupture, even when no trauma or unusual force is present.
Difference Between Disc Rupture and Herniation
A herniated disc typically describes a condition in which the disc nucleus is still contained in the outer wall, but is bulging asymmetrically. This is also sometimes referred to as a& contained herniation or closed disc herniation.
A ruptured disc means that the nucleus is no longer contained within the disc wall. However, it does not mean that the nucleus has leaked out of the disc. Some ruptures entail tiny holes in the annulus, preventing significant amounts of nucleus material from escaping. Other ruptures allow some nucleus material to leak from the disc. Finally, severe ruptures might allow the entire nucleus to exit the disc structure, occasionally under pressure.
Ruptured Disc Causing Chemical Radiculitis
Chemical radiculitis is a process by which the glycoproteins which comprise the nucleus pulposus irritate the surrounding spinal nerve roots if they leak out of the annulus fibrosus.
In the case of disc rupture, the nucleus material exits the disc, sometimes under force, and might come into contact with the nerve roots at that vertebral level. This irritation is believed to cause pain and related neurological symptoms which might last until the proteins are neutralized or absorbed by the body. This is a controversial theory and is not accepted by all care practitioners. Additionally, some patients might be more prone to developing chemical radiculitis than others, due to heightened genetic neurological sensitivity.
Spinal Disc Rupture
I have a good idea about herniated and ruptured discs, since I have some of each. My L4/L5 is badly herniated towards my spinal cord, while my L5/S1 ruptured long ago. I also have 10 other contained herniations in my neck and upper back which were more recently discovered. That makes a total of 12 herniated discs for me.
For many years, my back pain was blamed on the lumbar disc abnormalities and I accepted that diagnosis 100%. I suffered for 18 long years until I discovered the truth about the common and typically asymptomatic nature of most herniations and ruptures. Sure, these events can certainly be painful for a time, but rarely cause the kind of long-term chronic disc pain syndromes often blamed on them in the majority of diagnosed patients.
If you have suffered a disc rupture, make sure to understand the complete objective facts of the condition. If you simply accept that a bulging or broken disc is the exclusive cause of your pain, without demanding clinical symptomatic correlation, statistics clearly demonstrate that you are likely to continue suffering for many years to come.





