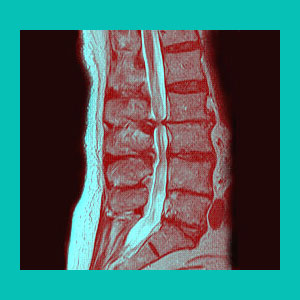
Herniated disc diagnosis is a fairly straight forward process clinically, but many processes are not performed correctly, leading to poor treatment outcomes. Diagnosis entails a confirmation of the existence of a disc herniation in the spine, as well as a comprehensive prognosis for how the condition might affect the individual in the future. While disc abnormalities are easily visualized using diagnostic imaging, correlating symptoms to them is a far more involving process. Errors are unfortunately all too common when it comes to linking disc bulges to back, neck and sciatica pain.
In this article section, you will find focused discussions relating to the diagnostic process for intervertebral disc herniations.
Herniated Disc Diagnosis Fallacies
Some care practitioners claim to be able to diagnose a disc herniation merely by touch or feel. Some also claim they can diagnose the condition with a simple physical exam and range of motion test. The often agonizing straight leg raising test is a common ridiculous example of a diagnostic test which proves absolutely nothing at all. These methods might be part of a full diagnostic procedure, but are not an accurate means of positively identifying any back pain syndrome, including bulging or ruptured discs.
Do not put your faith in any herniated disc diagnosis which has been accomplished through any of these means. Make sure to insist on an MRI study to confirm the presence of a herniation, as well as to visualize the exact effects which might be produced on the surrounding spinal nerve tissues.
Learn more about the common misdiagnosis of herniated disc nerve damage.
Bulging Disc Diagnostic Topical Essays
Read the following discussions to learn more about the diagnostic process for intervertebral herniations.
A disc impinging on the thecal sac is usually not a symptomatic occurrence.
A disc abutting the spinal cord may or may not produce some form of symptomatic expression. However, a disc compressing the spinal cord is virtually always a painful and dangerous health issue, since it causes herniated disc spinal stenosis.
A herniated disc compressing a nerve is usually enacted through the process of neuroforaminal stenosis.
Getting a second opinion on a herniated disc is always a good idea before pursuing any form of treatment.
Misdiagnosed herniated discs are different than misidentified herniations. Misdiagnosed bulges truly exist, but are not the source of pain.
Other Diagnoses Related to Herniated Discs
In addition to a herniated disc, there are many other independent or related diagnoses which might be discovered in the patient’s spine:
Pinched nerves might be created by intervertebral herniation or from many other structural issues within the vertebral canal.
Sciatica is a common result of lumbar herniations.
Chemical radiculitis describes chemical irritation of nerve fibers from leaking disc nucleus proteins.
Cauda equina syndrome denotes a medical emergency in which the grouped lumbar and sacral nerve roots are compressed in the lower spinal regions.
Foraminal stenosis happens when the openings through which the nerve roots exit the vertebral canal lose patency. Lateral recess stenosis is a similar condition that describes a reduction in the available space on the approach to the neuroforaminal openings.
Spinal stenosis, also called central canal stenosis, describes a scenario when the spinal cord or cauda equina is impinged upon by a narrowing of the vertebral canal.
Ligamentum flavum hypertrophy is a soft tissue problem that can reduce the effective size of the central spinal canal and might lead to other concerns, such as ligamentous ossification.
Herniated Disc Diagnosis Modalities
The only way that a herniated disc can be accurately diagnosed is with a detailed soft tissue imaging study, such as an MRI, CT scan or myelogram. The myelogram is the least effective method, while the CT scan is adequate. The best method of visualizing a herniated disc is using the advanced technology offered by the MRI.
X-rays will not be able to diagnose a herniated disc in most cases. X-rays will simply show disc height in relation to the vertebral bones and are often used for diagnosing degenerative disc disease, as well as any herniation condition. Truthfully, X-rays should not be used to diagnose any soft tissue condition or injury.
Spinal discography is a separate diagnostic test that is used to correlate pain to a suspected intervertebral source. However, discograms have many risks, so patients must think carefully before undergoing the test.
Read our full coverage of the entire range of herniated disc tests.
Herniated Disc Diagnosis Nocebo Effect
The diagnostic procedure is far more involved than simply identifying the existence of a herniated disc. In fact, that is the easiest and least important facet of the procedure. The most critical aspect of the diagnosis is how the news is presented to the affected patient. This is where doctors can create or negate the possibility of a chronic back pain syndrome, simply by their choice of words.
If the doctor informs the patient the real facts about disc herniations and how they are common, widely experienced and rarely problematic, the patient will be placed on a course towards true recovery. Even painful disc conditions will typically resolve when treated with this simple diagnostic formula. However, this is not the usual approach taken by the majority of caregivers. Far more common is something more like this:
You have a herniated disc in your spine. This disc is pressing on some nerves and is causing you severe pain. This is a serious condition and will require ongoing and treatment and possibly even surgery. I want to see you again, next week so that we can set up a therapy plan. Until then, stay in bed and don’t move.
This approach will create pain where none exists, worsen and perpetuate pain that already exists and intensify general anxiety, fear and psychosomatic implications of the condition. In essence, this diagnostic method does exponentially more damage than the actual herniated disc could ever do on its own. This is called the nocebo effect.
Be sure to question your doctor about your herniated disc prognosis after learning that you have an intervertebral problem and demand answers which make sense… Actual sense, not just economic sense to your care provider.
Guidance on a Herniated Disc Diagnosis
Most importantly, do not allow any doctor, therapist or chiropractor to convince you that you have a herniated disc without proper diagnostic imaging studies.
Second, do not buy into the hype surrounding the herniated disc diagnosis. The majority of disc herniations do not cause any pain at all. Those which are initially painful can heal, even without any medical treatment.
Third, if your doctor tries to convince you otherwise and pushes you into some drastic treatment option prematurely, consider finding a new doctor.
Obviously, all herniations are case-specific and highly individual conditions. Some disc herniations can present severe symptoms, such as cauda equina syndrome, but it must be known that these are the extreme minority of cases. If you have a medical emergency due to a disc condition, there will be no doubt.
If you have doubt, stick to the above advice and treat the condition conservatively. Most of all, continue to learn about herniated discs and how they are really just another ultra common occurrence in the life cycle of a typical human spine. Learn more about the difference between a bulging disc and a herniated disc.
Learn to prevent the misdiagnosis of herniated discs while simultaneously effectively ending your pain using our proven and peer-acclaimed Cure Back Pain Forever Program.






