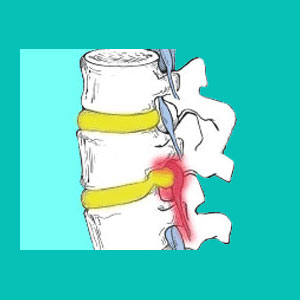
A herniated disc compressing a nerve is a common diagnosis used to explain a variety of back, neck and limb pain symptoms. It is also the most prevalent suspected source of sciatica in the legs and many radicular pain conditions in the upper body, as well. There are facts and myths regarding compressed nerve conditions which should be understood by any affected patient. Of all the theorized causes of herniated disc pain, pinched nerves are certainly one of the most commonly misdiagnosed.
This investigational article will look at how a pinched nerve can come about from a bulging disc. We will explore the symptoms which might be produced, as well as some common misconceptions of compressive neuropathy conditions.
Herniated Disc Compressing a Nerve Explained
There are 2 main sources of pinched nerves which may be enacted by a herniated or ruptured disc:
Foraminal stenosis is a result of disc prolapse which completely or partially blocks off the neuroforaminal space. This is the opening through which the spinal nerve roots must pass and is the most common location for actual pinched nerves to occur. This condition can occur at virtually any spinal level, affecting the nerve serving a specific and well defined set of muscles on one side of the body.
Central spinal stenosis and lateral recess stenosis can pinch one or more nerves in the lower back, since the spinal cord has already separated into the cauda equina structure. In cases of severe central stenosis, a nerve root may be compressed before it even branches off the cauda equina grouping.
Herniated Disc Nerve Compression
In cases of lumbar central spinal stenosis which are deemed to be compressing a nerve root, the chance for misdiagnosis is fair. If the nerve can be clearly visualized as being compressed, then the chances decrease greatly, but in many patients, this is not the case. Many patients have coincidental disc abnormalities or simply demonstrate a narrowing of the central canal. These condition may not be symptomatic at all.
For foraminal stenosis sufferers, the chance for misdiagnosis is much higher. The space through which the nerve must pass must be almost completely blocked for the disc to have any significant and lasting effect on the nerve root. When the disc is simply touching the nerve root, there is generally not anything to be concerned with, but actual pressure enacted against the root may be a problem. In most cases, the nerve root is not visualized as being compressed, but the foraminal space is said to be narrowed, which is a normal part of the aging process anyway and is not inherently symptomatic.
Herniated Disc Compressing a Nerve Solutions
When a single nerve root is compressed, left side or right, there will be very predictable neurological outcomes, including true objective numbness and weakness in a specific and defined muscle location or set. Subjective symptoms are the norm for most herniated disc patients and few demonstrate these objective neurological patterns, despite active diagnoses of pinched nerves.
The biggest myth is that a compressed nerve will cause chronic pain, but this is not a reality at all. Continued compression causes a nerve to stop signaling altogether, enacting a lack of sensation, not acute or chronic pain. Remember to keep this information in mind as you go through the herniated disc treatment process.
Herniated Disc > Herniated Disc Diagnosis > Herniated Disc Compressing a Nerve




