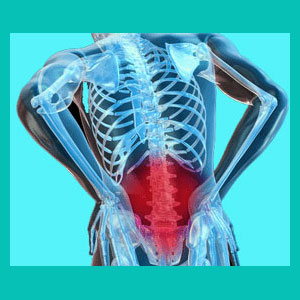
Chronic herniated disc pain can make any acute disc pain condition into a long-term agonizing ordeal. Chronic pain consists of symptoms which go one and on, despite active medical care. These types of stubborn pain conditions can literally take away the will to live in some patients and always have inherent emotional consequences on all they touch. Chronic back pain laughs in the face of medical treatment, defies surgical intervention and has become one of the most prevalent health crises in existence today.
This article will profile what it is like to live with chronic herniated disc pain. We will explore why symptoms can become a lasting concerns and how most patients are terribly mismanaged within the medical system.
Chronic Herniated Disc Pain Explained
Chronic back pain is an epidemic condition which affects a substantial percentage of adults and even some children. Chronic symptoms can be caused by a vast number of different diagnosed conditions, but is most commonly blamed on a herniated disc. Ironically, this spinal abnormality is found in many people who do not experience any back or neck ache and is a coincidental occurrence in many patients who do endure horrific chronic symptoms.
Herniated discs have a fearsome reputation, based on mythologies and diagnostic nocebo, but the reality of mild and moderate bulging discs shows them to be mostly innocent and asymptomatic. In essence, this common condition might create short-term pain in some patients, but is seldom responsible for the creation of unrelenting suffering. The exception to this rule is when the disc is verifiably causing some neurological problem, such as in the case of central spinal stenosis. In these scenarios, chronic pain may be both expected and logical, given an extreme disc pathology.
Chronic Disc Pain Mechanics
Chronic disc pain rarely occurs due to the same conditions responsible for acute pain. Acute symptoms often result from injury and heal within an expected time frame, as is the body’s natural design. Chronic symptoms often defy logic and persist even when no definitive cause is apparent.
Some chronic symptomatic concerns are not linked to a particular injury or degenerative concern, but instead are driven by an ischemic process tied to the interaction between the emotional mind and the physical body. This type of pain is called psychosomatic (also called psychologically-induced or psychogenic) and is a literal epidemic in the modern healthcare system. Some great misconceptions about psychosomatic disc pain are that it is imaginary or exaggerated in most patients.
The reality of psychosomatic pain is quite the opposite. Psychosomatic describes verifiable pain which exists in the physical body, but is derived from a psychoemotional process, not an anatomical injury or structural condition. What this means is that the symptoms are as real as any other pain, but the source is emotionally driven, not anatomically related.
Some patients had an injury which healed, but a mindbody pain syndrome took over, seemingly perpetuating pain from the original trauma. Other people with psychosomatic pain have no physical basis for their symptoms at all, but suffer greatly.
Medical science does not typically diagnose mindbody concerns, so the pain is generally misdiagnosed as coming from one of many back pain scapegoats, such as a herniated disc.
Of course, it is possible to have persistent pain from a purely physical reason, but it is rare. The overwhelming majority of disc pain events resolve in 2 to 8 weeks. Nerves, which are definitely compressed by a herniated disc, do not cause ongoing pain; they cause numbness, since they cease signaling completely in a short time.
Patients who continue to experience pain for months or even years, are likely to be suffering from one of 2 possible scenarios: First, an undiagnosed structural issue may exist elsewhere in the spine and is the actual cause of pain. Second, a psychosomatic source may exist, or there may be a psychosomatic perpetuation process, if the patient did indeed suffer an acute disc injury at one time. Don’t forget, psychosomatic conditions often carry on physical symptoms in a location which was the site of a previous injury. This makes the syndrome all the more convincing.
Chronic Herniated Disc Pain Considerations
The amount of patients worldwide with chronic herniated disc pain numbers in the hundreds of millions. It seems there is no helping these poor souls using appropriate medical, complementary or even surgical interventions. Their pain continues year in and year out, without getting any better. While most of these patients question the effectiveness of their treatments, virtually none consider the validity of their diagnosis.
This is the reason why so many herniated disc patients never get better. They are simply pursuing treatment for a condition which is not even responsible for their pain. Yes, they have a herniated disc. So what? So do I (12 actually). So do many people without pain.
The disc is not the cause of the symptoms; it has merely been blamed for them. This fact has received a huge boost of support from recent diagnostic protocol changes enacted by major medical associations. These alterations caution doctors never to implicate a spinal abnormality as the source of pain, unless a verified pathological process can be proven. Research goes on to say that few mild to moderate disc irregularities demonstrate a pathological component, now or ever.
Discover the actual cause of the pain and you will have found your cure. It is that simple. If you are still resistant to the idea that an alternate structural or even psychosomatic process might be at least partially responsible for your chronic herniated disc pain, then you must really want to hold on to the suffering.
I know that when this idea was brought up to me, I was receptive to the theory, since I was desperate for a cure. I have 12 herniations at this point and only a few might have the potential to cause pain, yet none do. The rest of these disc protrusions fit the typical profile of just existing, but not causing any pain whatsoever.
Herniated Disc > Herniated Disc Pain > Chronic Herniated Disc Pain





