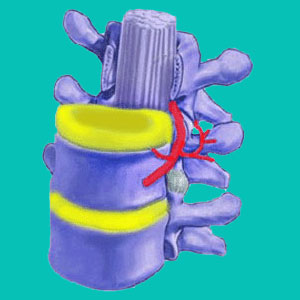
An intervertebral disc protrusion is another diagnostic term for a herniated disc. Protrusion is a term usually reserved for significant disc bulges, in which the herniation extends past the normal boundaries of the vertebral bones. Most protrusions are not problematic and might even shrink back considerably on their own. However, some protrusions might affect the spinal nerve roots or even impinge on the actual spinal cord itself, enacting painful, although usually temporary symptoms.
This article will focus on spinal disc herniations which are diagnosed as protrusions. We will separate fact from fiction when it comes to disc diagnoses and explore how symptoms can be enacted when nerve tissue is affected.
Disc Protrusion Condition
A protrusion occurs when the outer disc wall is severely compromised, allowing the interior nucleus pulposus to project into a pocket or bubble formed on one side of the disc. This distention usually does not alter the function or integrity of the overall disc structure, but will place the disc under greater risk for rupture.
A protrusion in the disc is what is typically blamed for placing pressure on spinal nerve roots or the thecal sac, which surrounds the actual spinal cord. While this does happen in some instances, it is diagnosed far more often than it actually occurs. Just because the herniated disc material touches the thecal sac, does not mean that any significant or even noticeable spinal stenosis symptoms will result.
Additionally, the common diagnosis of foraminal stenosis due to a herniated disc is actually quite rare, but is blamed for a huge number of back pain complaints every year. It is no wonder that most of these poorly diagnosed conditions do not respond well to even the most appropriate and indicated herniated disc therapy modalities.
Protruding Spinal Disc Solutions
Many times, disc swelling will subside without any treatment. Often, all the condition requires is some time and home-based care to fully heal. Other times, the condition will remain permanently, but will not cause any pain. If pain was produced early in the herniation event, it will usually alleviate within 2 to 8 weeks, even without medical care.
Occasionally, verified herniated disc pain might become a chronic concern and may require drastic medical treatment. Even less commonly, a herniated disc will cause sudden neurological concerns, such as cauda equina syndrome, which typically require immediate surgical intervention.
Disc Protrusion Editorial
If you have a protruding disc, join the group. There are billions of us all around the world who have disc abnormalities in our spines. Herniated discs are not usually the nightmarish tormentor portrayed by the back pain industry. They are quite common and well tolerated by humans, since the birth of our species.
The human spine has evolved to improve, not fall apart. Herniated discs do not have a significant place in medical history as the source of chronic pain. The high incidence of chronic and debilitating back pain did not occur until about 70 years ago.
Did our species suddenly develop an amazing susceptibility to the current epidemic of back pain? Or, is dorsopathy just another of the multitude of chronic pain conditions which have been fostered by the medical industry and actually imposed upon patients through the diagnostic nocebo effect?
You can be the judge once you know the facts for yourself.





