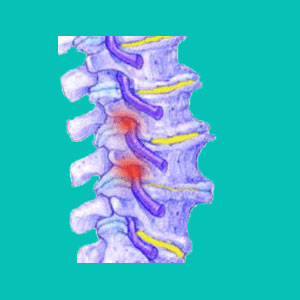
Spinal foraminal stenosis is the narrowing of the typical neuroforaminal spaces between the vertebrae. The spinal nerve roots exit through these same openings and when the stenotic change is severe, these neurological structures might suffer compression and subsequent dysfunction. When a nerve root is constricted, this is commonly known as a pinched nerve.
This diagnosis is controversial, since in many instances, the nerve is not definitively compressed in any way, but instead may only be touched by whatever process or structure is causing the narrowed foramen. However, when compression does truly occur, serious symptoms, such as sciatica, may occur.
This essay will investigate the cause of foramen narrowing and the effects these stenotic changes will potentially have on the exiting nerve roots. We will also discuss the reasons why foraminal stenosis is often coincidental to any symptoms which may be experienced in patients who do not receive proper neurological evaluation and correlation.
Foraminal Stenosis Definition
Nerve roots branch off the spinal cord and cauda equina at every vertebral level and leave the spinal column through the openings in between the individual vertebral bones. These openings are called foramen or neuroforamen.
Nerve roots are main conduits of neurological activity between the spinal cord and the rest of the body. If one of these nerve roots is compressed, as it passes through the foraminal opening, the condition is called a compressive neuropathy or pinched nerve.
Causes of Foramen Stenosis
While there can be many causes for stenosis of the foramen to occur, there are 2 predominant reasons in the majority of patients:
Herniated discs can bulge into the foraminal opening, compressing the nerve root against the wall of the neuroforamen. This is sometimes called nerve compression, nerve impingement or nerve constriction. This condition is very commonly diagnosed, but is actually often an incorrect symptomatic assessment. Nerve compression due to a herniated disc is rare and long-term pain from this occurrence seldom occurs.
Osteoarthritis is a normal process of spinal degeneration which affects most adults to one degree or another. Bone spur formation sometimes occurs and can be encouraged if the patient also has significant degenerative disc disease in the affected vertebral levels. If a bone spur forms close to the foraminal opening, it might encroach on the spinal nerve root, causing compression. This type of stenosis does occur in some patients and might require surgical treatment to resolve.
There are other less common congenital, developmental and trauma-related causes of stenosis of the neuroforamen. However, the above examples describe the conditions affecting most diagnosed individuals. It should be mentioned that foraminal stenosis often entails a combination of narrowing factors all working in unison.
Stenosis of the Neuroforamen
Just because the foraminal space is reduced does not mean anything pathological is occurring. No symptoms will be generated unless the nerve root is affected.
The symptoms of this condition depend greatly on the extent of the nerve compression and the location of the constricted nerve root. Typically, nerve pain is one of the first symptoms, but tingling, weakness and numbness are also common effects in the bodily region served by the affected nerve.
Sometimes, there are other effects enacted by a seriously compressed spinal nerve, which might affect motor ability of a body part or even some of the autonomic functions of a particular anatomical system. These effects can be very serious, especially when they occur in the upper cervical region, since these autonomic processes are vital to sustain life and health.
Foraminal Stenosis Conclusions
Stenosis of the neuroforamen due to a herniated disc is a very common diagnosis. It is typically made by looking at an MRI image where the herniation appears to touch the nerve in some way, shape or form. Many of these conditions are mistakenly identified, since most herniations do not actually cause pain, even if they occur close to a foraminal opening.
For accurately diagnosed nerve impingement from a bulging disc, the symptoms will usually resolve on their own, after the disc swelling has lessened with time. This will occur in 2 to 8 weeks of conservative care in most patients.
Patients with chronic herniated disc pain from a foraminal stenosis condition have a greater chance of being misdiagnosed. Research has shown that continuing nerve compression will cause the nerve to stop signaling altogether, creating a numb condition, not a painful symptomology. If chronic numbness exists, the diagnosis is likely to be correct.
If chronic intermittent pain exists, the nerve might only be partially compressed and the diagnosis may or may not be right. If chronic constant pain exists, the diagnosis is generally wrong and should be reconsidered carefully.
Many theorized nerve compression cases are actually innocent and the symptoms might be present due to an ischemic process using the apparent stenosis as a convincing means of explaining symptoms. For these conditions, I always recommend considering knowledge therapy as an alternative path to treatment.
For actual herniated disc-related structural nerve compression, I often recommend non-surgical spinal decompression, using the DRX9000 or other popular system.
For actual foraminal stenosis due to advanced arthritic change, there are some minimally invasive surgical procedures which can provide a clear pathway for the nerve and prevent future pain and related discomfort.
Make sure to research all your options thoroughly and always exhaust all conservative options before considering surgical intervention of any kind.
Spinal-Stenosis-Treatment .Org is the leading objective information provider for all things related to neuroforaminal stenosis and pinched nerves.
Herniated Disc > Herniated Disc Diagnosis > Foraminal Stenosis





