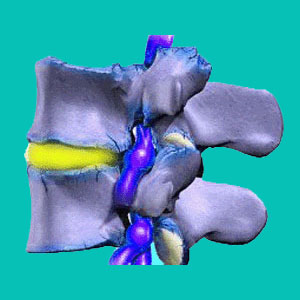
Neuroforamen are the openings in between the individual vertebra through which the nerve roots exit the spinal column. These structures are often blamed for being the source of ongoing neck or back pain syndromes, when a herniated disc or spinal arthritic process causes a reduction in the size of the opening, potentially creating a pinched nerve condition.
This article will explore how the neuroforaminal spaces can be affected by herniated and degenerated discs. We will also look at the facts and myths associated with pinched nerve roots in the spinal anatomy.
What are Vertebral Neuroforamen?
There are foraminal openings at every vertebral level. These structures are basically just small holes which allow the nerve roots to branch off the spinal cord and exit the spinal column to serve the autonomic, sensory and motor needs of the body. These openings are far larger than is required by the nerve roots, but can become smaller due to the accumulation of arthritic debris and bone spur growth, as part of the osteoarthritic process.
Atypical spinal curvatures, both side to side, like scoliosis, and front to back, like hyperlordosis, can reduce the patency of the foramen. Finally, herniated discs can also minimize the size of the foraminal spaces, especially in posterolateral varieties of prolapse.
Neural Foramen Facts
In order to experience a true pinched nerve condition, the foraminal opening would have to be virtually completely closed off. Although pinched nerves are commonly diagnosed, this situation rarely occurs, leading to widespread speculation about whether most diagnosed compressed nerves actually exist. In most cases, even a significantly narrowed foraminal opening will allow for perfect neurological functionality.
Remember, spinal degeneration is normal and expected. Spinal arthritic processes affect all of us as we get older. Bulging discs are also very common and rarely cause any ongoing pain or symptoms. Additionally, there is much debate as to whether disc material is even capable of compressing a nerve, unless it is definitely pressurized or calcifies.
Neuroforamen Pathology
Continued compression of a nerve will result in complete loss of neurological function. The result will be numbness, not chronic pain. Chronic nerve pain conditions blamed on herniated discs or osteoarthritis are very common, but are rarely correctly diagnosed. Far more typical for creating actual ongoing nerve pain is oxygen deprivation. Ischemia of the nerves can occur at very low levels of oxygen deprivation, causing wide ranging effects, such as pain, tingling, numbness or weakness.
If you have experienced chronic nerve pain from a diagnosed constricted nerve condition, consider your diagnosis and treatment options carefully. These pain syndromes commonly ignore appropriate treatment, due to the fact that the nerve is not compressed at all.
This is doubly true when the suspected cause of compression is a herniated disc. If this situation describes your circumstances, be very careful before you wind up enduring years of useless and unnecessary treatments, like I did, or even an invasive spinal surgery.




