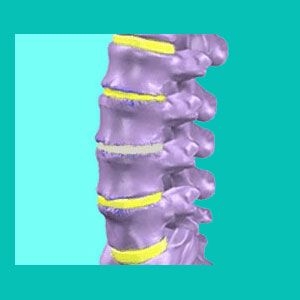
Intervertebral disc calcification describes a scenario in which part or all of an intact or damaged intervertebral spacer ossifies into a bony structure, instead of maintaining its natural soft and pliable consistency. There are many diagnostic terms associated with this condition including: calcified herniated disc, calcified ruptured disc, calcified disc, intervertebral calcification, calcified sequestration, ossification of an intervertebral disc or disc ossification.
Although the idea of a normally supple spinal disc transforming into a bony tissue sounds horrible, most cases are statistically asymptomatic. There are many possible causes and contributors to the ossification process in spinal discs, with degeneration, disease and injury being the most common.
This treatise delves into disc calcification and ossification processes that might affect normal, bulging, herniated or ruptured intervertebral disc tissues in the human spine.
What is Disc Calcification?
Calcification involves the loss of moisture in a soft tissue and the replacement of water with minerals, slowly hardening the structure and transforming it towards skeletal rigidity.
Intervertebral discs consist of 2 components, the outer fibrous wall, called the annulus fibrosus, and the inner center, called the nucleus pulposus. The annulus is a durable, multi-layered shell that contains the nucleus and provides strength to the disc tissue. The annulus can harden, but this is uncommon. The nucleus is a moisture-rich core with a natural consistency of a thick jelly. As the disc desiccates, minerals might be deposited into the interior of the disc, hardening the soft center into a firm and inflexible mass.
Ossification can occur in degenerated discs that decrease in mass due to water loss.
Calcification can occur in bulging discs, encompassing part or whole disc structures.
Calcification can also affect herniations, once again affecting either the distended aspect of the disc, the normal unaffected part of the disc or the entire disc structure.
Calcification might also occur in areas of a ruptured disc, most often affecting the nucleus tissue that is ejected from the annulus. Of course, if this tissue migrates and becomes a sequestered disc, then ossification can also occur, leaving small fragments of bony tissue throughout the neighboring regions of the spinal anatomy.
Calcified Spinal Disc
There are many possible causes and contributors to intervertebral calcification within the backbone. Some of the most common sources include any or all of the following factors:
Disc degeneration is the most common reason to explain ossification of the spinal spacers. It is completely normal, expected and universal for adults to lose moisture in their discs, particularly those in the mid to lower lumbar levels and those in the mid to lower cervical levels. Desiccation of disc tissue can leave discs weak and susceptible to mineral deposit formation.
Disc injury can cause intervertebral bulging, herniation or annular tears. All of these factors, combined with age and activity-related wear and tear, can increase the risk of developing intervertebral ossification.
Certain disease processes might factor into the development of ossified intervertebral discs. These include from extreme osteoarthritis, ankylosing spondylitis, rheumatoid arthritis, gout, acromegaly, polio, amyloidosis and osteopenia.
Dietary or metabolism disorders can predispose some anatomies towards calcification conditions in the spine or elsewhere. These might include alkaptonuria and haemochromatosis.
Genetic predisposition can take many forms and might make some people far more prone to the development of ossification of various soft tissues, including the spinal discs and spinal ligaments.
Consequences of Disc Calcification
When degeneration is to blame for calcification in an otherwise normal disc, the condition is virtually always asymptomatic. The patient might lose some degree of mobility in the affected vertebral level, but no pain or neurological consequences should be expected, as long as the central vertebral and foraminal canals remain patent.
In cases of damaged, herniated and ruptured discs, calcification may or may not create symptoms. In these cases, the mechanism usually falls into one of two possible categories:
Calcified bulges, herniations and disc fragments might interfere with the actual functionality of spinal movement, possibly causing a crude form of mechanical pain syndrome. We see this most often with ossified disc fragments that migrate during an intervertebral sequestration event. These fragments can cause mobility issues in the various moving parts of the spinal anatomy.
More likely, the calcification might affect the functionality of nerve tissues, by impinging on the spinal nerve root or spinal cord at the affected level. Pressurized herniations and ruptures which calcify are uncommon, but may create difficult-to-resolve symptomologies in rare cases, often requiring surgical intervention.
Even when a herniation places pressure on a nerve structure, the soft and pliable nature of a typical disc will allow time alone to potentially resolve the compression condition. This is why many symptomatic herniated discs do not require treatment. However, once ossified, the disc swelling will not resolve with time, increasing the necessity for medical intervention when nerve tissue is influenced.
Spinal Disc Ossification
Calcification can affect many of the soft tissues in the body, including the spinal discs and spinal ligaments, such as the longitudinal ligaments or the ligamentum flavum. Calcification is not inherently symptomatic, but may produce striking and frightening looking results on diagnostic films. It is crucial for diagnosed patients to fully understand the nature of their particular ossification condition, and its potential effects on the surrounding spinal anatomy, before seeking any type of professional care or treatment.
Remember that just because back or neck pain is present, in conjunction with an ossified disc, does not mean that the disc is the source process. There might be many other plausible explanations for the symptomology. This is precisely why diagnosed patients should seek several professional opinions from a variety of neurologists and orthopedists before taking any one opinion as guidance towards surgery or other drastic intervention.
Herniated Disc > What is a Herniated Disc > Disc Calcification






