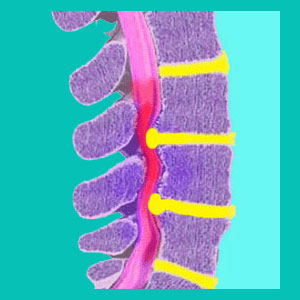
Herniated disc spinal stenosis is a diagnosis in which the patient is deemed to have a central canal which has been narrowed by a bulging or ruptured intervertebral disc structure.
Spinal stenosis can occur from many potential causes, including herniations, osteoarthritis, spondylolisthesis and scoliosis, among others, but herniated discs are one of the most controversial contributors known. This is because most true stenosis conditions are permanent and will not resolve without some form of invasive therapy. Intervertebral herniations, meanwhile, may decrease in size without any therapy, making this particular type of stenosis a possibly transitory circumstance.
This discussion focuses on transient stenotic conditions which are enacted by intervertebral pathologies.
Diagnosis of Herniated Disc Spinal Stenosis
It is quite common for a central disc herniation to impinge on the thecal sac which surrounds the spinal cord. It is also not unheard of for the disc to press into the actual cord or cauda equina itself. It is rare, however, for this effacement to create any serious pain or neurological symptoms, as long as there is no definitive compression of the spinal cord or cauda equina structures. Most herniations which enter the spinal canal do not do anything but exist there.
In some cases, especially when enacted by sudden and extreme trauma, a central or posterolateral disc herniation can create a symptomatic stenosis condition which can cause acute pain and other symptoms, including weakness, numbness and tingling in virtually any bodily location below the level of canal narrowing.
Treatment for Disc-Related Spinal Stenosis
Being that most mild to moderate spinal stenosis conditions are not symptomatic, especially when created by a soft tissue pathology such as a herniated disc, the majority of diagnosed patients will not require any specialized treatment. Usually professional monitoring of the issue is enough for minor stenosis events.
However, unneeded treatment is sometimes provided, since the condition is occasionally grossly misdiagnosed as being problematic, leading to symptomatic escalation via nocebo effect and a long line of failed therapy modalities.
Treatment for actual disc-related cord or cauda equina compression can often be successfully completed using spinal decompression, surgical intervention or simply waiting it out.
Herniated Disc Spinal Stenosis Experiences
Just within the past few years, I was diagnosed with many previously unknown herniations in my neck, including one particularly troublesome looking one at C6/C7. I was shocked to see how this herniated disc was pressing so far into my spinal cord and was immediately concerned with the possibility of cervical spinal stenosis.
These herniations were obviously present for a very long time, since the usual degenerative changes were in full effect around the bulging discs, proving that I had been active for so many years with these cervical irregularities without even being aware that they existed. This made me feel a bit better, but I continue to get this one really bad prolapse monitored regularly just to be sure it will not become a serious health concern.
Herniated Disc > Herniated Disc Diagnosis > Herniated Disc Spinal Stenosis




