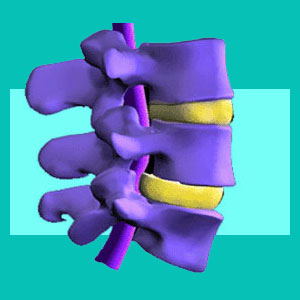
Learning all about herniated discs is crucial for anyone diagnosed with disc-related back, neck or sciatica pain. The intervertebral discs have the dubious distinction of being blamed as the source of more back pain occurrences than any other reason. While it is true that herniated discs can create symptoms in some cases, ongoing pain is actually quite rare and should go away with or without any particular treatment. Many cases of chronic dorsalgia blamed on a herniated disc are misdiagnosed.
This essay will detail the basics of herniated discs. We will look into the causes of disc pathologies, as well as the implications of the diagnosis.
Why Learn All About Herniated Discs?
Spinal discs separate the vertebral bones, acting as shock absorbers for the anatomy and helping the preserve the curves inherent to the human spine. There is no doubt that the intervertebral discs are an important part of our spinal anatomies and they actually account for about one quarter of the total length of the spinal column.
However, spinal degeneration is also normal and expected. What is known as degenerative disc disease is certainly not a disease process at all, but instead, is a completely universal part of aging. It should also be noted that DDD becomes noticeable in the lumbar and cervical regions of most adults by the age of 30 and often times, much younger.
DDD and the other spinal aging processes, contribute to herniated discs, making these bulges and ruptures also a very typical part of a normal spine.
To simplify this section, the main point to remember is that mild to moderate disc prolapse is actually very common and may even be considered virtually normal in the lower lumbar and cervical regions by many doctors.
Herniated Discs Facts
While it is possible for a herniated disc to produce pain through various processes, including spinal stenosis, foraminal stenosis, chemical radiculitis and possibly discogenic pain, these events are not the rule. They are, in fact, the exceptions. Most herniated discs are not problematic or symptomatic. They are just there, doing no harm at all.
Herniations which occur due to spontaneous injury may certainly be painful for a time, usually 2 to 8 weeks, but should resolve without any particular treatment in most instances. Pain which lasts longer than this is rarely the result of any disc pathology, although this is exactly the diagnostic theory haunting countless patients worldwide.
Even when herniated discs are deemed to be symptom-generators, pain is not always the expected result. In fact, there are some disc diagnoses which elicit numbness or weakness instead of chronic pain.
About Herniated Discs Conclusions
Even painful herniated discs which do require treatment should get completely better with appropriate care. However, we all know that herniations have a nasty reputation as a stubborn and treatment-defiant condition.
The reason behind this is that back pain, as a rule, is sometimes misdiagnosed and therefore any subsequent therapy is doomed to fail before it even starts. No wonder diagnostic protocols were recently revised by some major medical associations for disc abnormalities. These changes inform doctors not to assume any disc irregularity located on diagnostic imaging is the source of pain, unless a definitive pathological process can be identified. It seems that modern medicine is finally catching up with research science for the first time in decades.
If you can not find relief from a herniated disc pain syndrome, I urge you to consider the obvious. Misdiagnosis is the most likely explanation and finding the real reason for the pain should become your top priority. Your spinal neurologist can prove very useful in successfully completing this quest for an accurate diagnosis.
Herniated Disc > Herniated Disc Facts > About Herniated Discs




