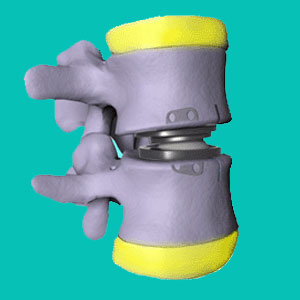
Disc removal surgery is a drastic option for particularly problematic and painful spinal discs. The trouble with removing a disc structure, partially or completely, is that now the spinal anatomy has been altered and this can definitely affect the surrounding vertebral levels, causing major effects on the health and functionality of the patient.
Disc removal also brings to mind the fact that a fully removed disc must be replaced with something, while a partially removed disc is now subject to accelerated degeneration and possibly a recurrence of the herniation. Overall, herniated disc surgery demonstrates disappointing curative results, regardless of the type of procedure selected. Disc removal is unfortunately no exception to this rule.
This dialog investigates the reasoning used to justify spinal disc excision, as well as the consequences of the surgical endeavor.
Full Disc Removal Surgery
Full disc removal is called a discotomy or full discectomy. This procedure takes out the offending herniated or degenerated disc and then stabilizes the spine using one of 2 possible procedures. The first and most common stabilization option is spinal fusion in which bone grafts and possibly surgical hardware are used to permanent fix the vertebral levels together, preventing the natural movement of the spinal bones. The second opinion is disc replacement surgery, using a synthetic intervertebral disc substitute, which will at least seek to maintain normal spinal function and individual vertebral level movement.
Discs can never simply be removed and the open intervertebral space left unattended. This would be a sure recipe for disaster.
Partial Disc Removal Surgery
Discectomy can also be used to remove only the herniated part of the disc, leaving most of the organic structure intact. This is the most common operative procedure for herniated discs, especially in first time surgical patients. Most doctors now perform minimally invasive versions of the procedure, commonly called microendoscopic discectomies.
Alternately, there are several minimally invasive procedures which do not cut away any of the disc at all. Instead, they use heat or radio waves to dissolve part of the nucleus pulposus, causing the bulging disc to shrink back closer to its original and asymptomatic state.
Of all the surgical procedures, these are perhaps the best options for many patients, since damage to healthy tissue is minimized and the disc has the best chance to heal fully without relapse. Of the 2 most common procedures used, I prefer the nucleoplasty approach to the more common IDET technique.
Removing a Spinal Disc Surgery
Whenever possible, it is best to avoid spinal surgery completely. Back surgery should be for emergency use only, since it demonstrates poor long-term curative statistics for most procedures and treated conditions.
Failed back surgery syndrome is a very real possibility, as well, making the risk substantial for most patients. It is generally accepted that patients should never undergo any type of surgery without first exhausting all conservative and noninvasive treatment modalities.
Many people can avoid surgery by investigating nonsurgical spinal decompression for intact disc herniations.
Most of all, if you do decide on surgery, choose your surgeon carefully and elect the least invasive type of procedure possible to speed your recovery and minimize the chances of a serious complication.
Herniated Disc > Herniated Disc Surgery > Disc Removal Surgery




