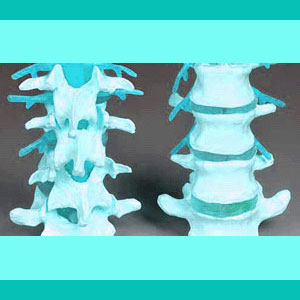
A herniated intervertebral disc is the most prevalent spinal abnormality and also the greatest villain in the back pain industry. Herniated discs are blamed for creating pain more than any other single spinal source. Disc pathologies are also the conditions most frequently treated surgically. Furthermore, herniations feature the absolute worst long-term curative results when treated with any type of spinal operation.
Herniated discs are incredibly common and most people may have several that they do not even know about. Although there is much concern about herniated discs, most of this is simply antiquated medical myth, misinformation and purposeful demonization of the poor maligned spinal disc for the sake of profit. Statistics clearly reveal that the majority of disc issues do not cause pain now or ever. However, there are times when disc bulges and ruptures can be painful; so it is crucial for patients to fully understand how a herniation may elicit symptoms when they are positively diagnosed.
This essay provides a factual and objective look at spinal disc herniations.
[contentblock id=1]
Herniated Intervertebral Disc Conditions
When a herniated disc occurs, the 2 structures which make up the disc anatomy will both suffer some change which is deemed to be irregular compared to a typical healthy spinal disc:
The containing disc wall, called the annulus fibrosus, may develop a weak spot and bulge outwards. This is the most common of the herniation profiles. This outer disc wall can also develop a hole, known as an annular tear, or can completely rip open, causing a disc rupture, also called an extruded disc.
[contentblock id=18]
Meanwhile, the soft disc center, called the nucleus pulposus also suffers a change in normal anatomical shape and symmetry. This jelly-like core can bulge into the weak spot in the disc wall, forming a pocket of nucleus material. The nucleus proteins can slowly or spontaneously leak or explode out of the outer wall in the case of a ruptured disc. If these nucleus pieces separate from the disc structure, it is called a sequestered or fragmented disc, depending on the number and size of the loose fragments.
Herniated Intervertebral Disc Diagnosis
No matter what occurs to change the anatomy of the disc structure, no direct pain will be ever felt by the disc itself. This is due to the simple fact that a spinal disc does not have blood vessels or nerve tissue in its interior. It is fed by small nerves and blood vessels in the cartilaginous endplates which attach the disc to the vertebrae above and below.
Symptoms from a herniated disc are blamed on one of 4 possible processes. Spinal stenosis is the most serious, while foraminal stenosis is more commonly diagnosed. Chemical radiculitis and discogenic pain are both controversial diagnoses and may not even affect most patients who experience the anatomical circumstances theorized to be responsible for causing symptoms in some tumor necrosis factor alpha-sensitized people.
Prolapsed Intervertebral Disc Considerations
I know how scary the herniated disc diagnosis can be. The very words can strike fear into the heart and soul and make a patient feel as if life, as they know it, is over. This is simply not true.
[contentblock id=10]
Learn the facts about herniated discs and see for yourself that most disc abnormalities are nothing to fear and are not likely to be the actual sources of chronic back pain, neck pain or appendage pain.
Although disc abnormalities are implicated in causing or contributing to many agonizing complaints, the horrible curative statistics of most herniated disc treatments prove that misdiagnosis is rampant in the back pain sector.
Clinical research from countless studies suggests that the majority of patients seeking a cure for disc pain are simply chasing after a specter. The disc is just not the real causation of their ongoing pain.
It should be noted that some herniations can be symptomatic and may even produce terribly afflictive expressions. However, these represent the gross minority of all diagnosed disc issues and will also usually respond favorably to appropriate care.
[contentblock id=2]
Herniated Disc > Herniated Disc Facts > Herniated Intervertebral Disc



