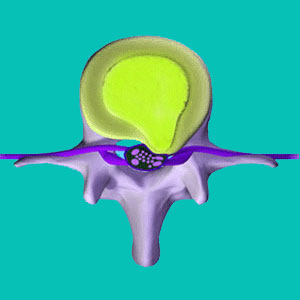
A posterolateral herniated disc is a very common type of intervertebral prolapse condition in which the herniated section of the disc is concentrated on one side or the other of the disc center. Posterolateral conditions are sometimes known as lateral disc herniations, but this can be very confusing, since there are also far lateral herniated discs, which can also be known by the same terminology. As always, I caution patients that while it is crucial to understand the basics of your diagnosis, it does not mean that a particular type or location of herniation is inherently any more likely to produce pain than any other.
The scope of this article will explore the posterolateral disc diagnosis and detail exactly what effects are possible to suffer from various severities of bulging intervertebral spacers.
[contentblock id=1]
What is a Posterolateral Herniated Disc?
Posterolateral disc bulges occur towards the left or towards the right. The herniated portion of the disc does not generally place direct pressure upon the frontal surface of the thecal sac or spinal cord, but severe posterolateral bulges can certainly compress the frontal/side surface of either structure.
Most of these herniations wind up in the lateral recess, which is simply the name for the space on either side of the spinal cord. It is in these areas that the spinal nerve roots exist as they head towards the neuroforamen to exit the spinal column.
Other diagnostic terms for posterolateral herniations may include left sided herniated disc, right sided herniated disc or paramedian herniated disc.
[contentblock id=22]
Posterolateral Bulging Disc Facts
The lateral recess is typically large enough to accommodate even rather sizeable herniations without causing any particular problems for the spinal anatomy. Some truly huge or problematic herniations may impinge upon the spinal nerve root which exits at the affected level, causing what is known as a pinched nerve.
Paramedial herniations which block out the neuroforamen are also sometimes called foraminal herniated discs, although most are simply classified as posterolateral protrusions.
Posterolateral bulges, like virtually all herniations, are best diagnosed using MRI testing, although some other types of tests will reveal them, as well.
Managing Posterolateral Herniated Discs
When I see patients reading these more technical diagnostic pages, I am happy, since it gives me hope that these sufferers are taking a truly active role in their own care. Learning is free and is so easy with the power of the internet.
[contentblock id=18]
In fact, you can learn basically everything you need to decipher your own MRI within a matter of minutes, if you are good at searching. This is fantastic, since it empowers patients to assist their care providers in the quest for lasting herniated disc relief.
Just remember that no matter where your herniation may occur, central, far lateral, posterolateral, anterior or otherwise, the chances of it being the source of chronic and severe back or neck pain are slim, unless definitive nerve interaction is occurring. Most disc issues are not inherently painful and those which are typically resolve without any special care.
For discs which do require active medical treatment, true structural issues usually respond well. For patients who have been in treatment for ages and have tried everything without success, the most logical explanation is usually misdiagnosis. Mistaken diagnosis occurs in terribly huge numbers within the back and neck pain treatment sector.
[contentblock id=2]
Herniated Disc > What is a Herniated Disc > Posterolateral Herniated Disc



