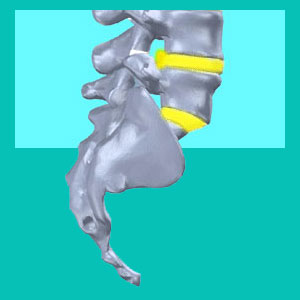
A prolapsed disc is an alternate diagnostic term for intervertebral disc herniation. Prolapse is a word which means to move out of anatomical position or to be displaced. While this is not exactly what occurs with a herniated disc, it is still a good description of what may occur to the disc nucleus during serious disc bulge or rupture events.
This article will describe the diagnosis of disc prolapse. We will look at why discs suffer herniation, as well as why some disc abnormalities may be completely innocent and coincidental to any pain which may exist in the regional spinal anatomy.
[contentblock id=1]
What is a Spinal Disc Prolapse?
Disc prolapse describes a situation when the interior of the disc, called the nucleus pulposus, bulges against a weakness in the outer disc wall, called the annulus fibrosus. This bulge might be minor and barely noticeable or might completely change the cosmetic shape and functional performance of the disc. Occasionally, the outer disc wall develops a rip, which is called an annular tear.
When the outer disc wall is completely compromised, the interior nucleus will often spill out into the surrounding spinal tissue. This is often referred to as a ruptured disc.
[contentblock id=17]
Prolapsed Disc Event
A disc can prolapse for 2 main reasons. Disc degeneration is a completely normal process which occurs in every adult as they age. Degeneration causes discs to dry out, losing precious moisture and becoming worn and brittle. Older discs are more likely to suffer annular tears and asymmetrical bulging, but are less likely to experience symptomatic herniations or ruptures, since the interior of the disc is now smaller and under less pressure, due to its dehydrated state.
Traumatic injury can cause any disc to spontaneously herniate or rupture. These circumstances can be rather painful, but are likely to resolve within 2 to 8 weeks statistically.
The majority of herniated disc concerns will not require any drastic treatment. Many will heal with no herniated disc treatment at all. Others may never heal, but are not the source of any pain, so their irregular anatomical condition is a nonissue.
Prolapsed Disc Guidance
Disc prolapse is one of the main scapegoats used throughout the medical industry to explain chronic back pain. However, research has shown that disc injuries can certainly be painful at first, but typically do not create long lasting pain complaints.
[contentblock id=16]
Every patient who is diagnosed with a disc prolapse condition owes it to themselves to understand exactly what is going on in their spines. If diagnosed, you must ask relevant questions of your doctor and be sure to receive clear answers which make sense to you.
Do not rush into any treatment option, unless you are faced with a dire predicament, such as cauda equina syndrome. Instead, it is best to explore all your options and always exhaust conservative therapy modalities before even considering any invasive measures.
Remember, disc surgery often demonstrates abysmal results for resolving chronic back or neck pain, even when the surgical goal of reducing the severity of a herniation is successfully met. Do not let any doctor push you into premature surgery, unless it is truly a medical emergency.
[contentblock id=2]



