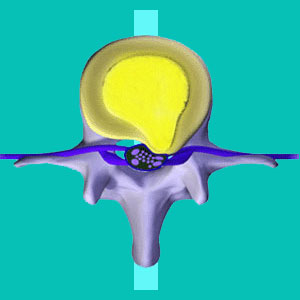
An extruded disc is also sometimes called a transligamentous disc, or more commonly, a ruptured disc. This disc profile entails a partial migration of all or part of the nucleus out of the annulus. Disc extrusions represent a minority of herniations, compared to the more common bulging disc profile.
Symptoms and treatment options for ruptured discs can vary somewhat from contained disc herniations. Therefore, it is crucial to understand the nature of every type of herniation before deciding on the ideal path to care.
This discussion will focus on disc extrusions and will detail the differences from other more common varieties of intervertebral herniation.
[contentblock id=1]
Extruded Disc Explanation
Ruptured discs typically begin as simple bulges and escalate to split open due to degeneration or traumatic injury. However, it is possible for a normal and healthy disc to undergo a sudden extrusion from extreme and focused injury, such as a car accident.
A disc bulge describes a condition in which the outer annulus fibrosus remains intact and free from annular tears. In an extrusion, the outer annulus rips open, allowing some of the softer nucleus pulposus to spill from the disc structure. In a true extrusion, the leaking nucleus material remains attached to the disc. Meanwhile, when the fragment breaks completely free and migrates away from the disc structure, completely losing contact, it is called a sequestered disc.
[contentblock id=11]
Basically, a rupture describes a general condition in which the inner core manages to break through the outer wall, compromising the structural integrity of the entire disc.
Disc Extrusion Causing Chemical Radiculitis
Besides potentially causing any of the usual nerve compression syndromes, including spinal stenosis, foraminal stenosis or pinched nerve conditions, extrusions also escalate the risk for chemical radiculitis. This controversial diagnosis seems to affect some patients with disc extrusions, but not others.
The inner disc nucleus is composed of proteins which might have an irritating effect on some surrounding neurological tissue. This can cause pain which might be quite severe in some patients. Luckily, specific forms of effective epidural injection therapy have demonstrated good curative results for confirmed cases of chemical nerve pain.
Just remember that this diagnosis is also a typical scapegoat for unexplained back pain and in these cases, the rupture condition itself does not seem to create any ill effects in the affected patient. Ruptures are not inherently linked to the incidence of symptoms any more than other varieties of herniation.
Extruded Disc Analysis
Ruptured discs seem to be worse than merely bulging discs upon first observation. However, this is not always the case. While ruptures can cause severe pain in some patients, they might also help to relieve pain in others.
[contentblock id=10]
A minority of disc pain sufferers actually endure a pinched nerve condition from a bulging, but intact disc. Sometimes, when the disc ruptures, it actually relieves pressure off the nerve tissue, ending the pain. Additionally, the ruptured disc material can calcify, sometimes supporting the compromised intervertebral level and providing some measure of lasting relief for the patient.
It is crucial to remember that disc conditions rarely cause the type of extreme or lasting pain they are often blamed for. In many cases, the disc is completely innocent and in other cases, the painful disc only enacts symptoms for a short time.
Lasting pain beyond the normal healing phase for a disc bulge may be the actual result of another structural or nonstructural source process, such as regional ischemia which may be linked to the diagnostic nocebo effect of the original disc condition.
[contentblock id=2]



