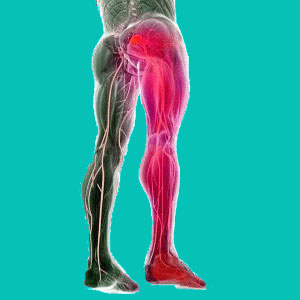
Herniated disc leg pain is a possible side effect of herniations in the lumbar and lumbosacral spinal regions. The lumbar intervertebral levels contain the nerve roots which eventually go on to form the sciatic nerve at levels L4, L5, S1, S2 and S3.
Leg pain and related neurological symptoms such as tingling, weakness and numbness are commonly blamed on bulging discs, but might be enacted by a variety of other causative conditions, as well. It is crucial to understand that research shows little, if any, correlation between herniated discs and chronic lower back pain. This is why it is essential to consider possible alternative explanations for leg symptoms which may result from atypical spinal curvatures, vertebral displacement, arthritic alteration and even nonstructural processes, such as oxygen deprivation.
This essay explores the many possible reasons why leg pain might be experienced in relation to a protruding intervertebral disc.
Sources of Herniated Disc Leg Pain
The usual diagnoses used to explain leg pain are certainly degenerative disc disease and herniated discs in the lumbar region, typically at L4/L5 or L5/S1. These intervertebral levels are almost always degenerated in adults by the age of 30 and sometimes much younger.
It is known that degenerated discs are more prone to suffering a herniation, so it is quite typical to find both varieties of these spinal abnormalities in the lower lumbar spine.
Other commonly diagnosed sources of leg pain include piriformis syndrome, sacroiliac pain and ischemia. Sometimes these conditions are really responsible for the pain, while the herniated or degenerated disc is simply a coincidental scapegoat. It is imperative to remember that central spinal stenosis anywhere in the backbone can cause pain and neurological dysfunction in the legs. This is rarely considered when moderate to severe disc issues exist in the lumbar spine. In most cases, an assumption is made that these lumbar discs are the symptomatic source, leading the patient far off course when it comes to finding effectual therapy. This is iatrogenic error in its purest form.
Leg Pain Caused by Herniated Discs
In order for a herniated disc to cause leg pain, it will need to compress a spinal nerve root, which is called foraminal stenosis. Alternately, if the disc bulges directly into the spinal cord or cauda equina, as a whole, this is called spinal stenosis.
While both of these occurrences are possible, they are diagnosed far more often than they truly occur in symptomatic form. Many herniations theorized to enact spinal stenosis are barely touching the thecal sac which surrounds the nerve structures. This rarely causes any pain or related symptoms. Likewise, many herniations thought to create foraminal stenosis might enter the neuroforaminal space, but do not compress or pinch anything.
Only a small percentage of diagnosed patients actually suffer symptomatic versions of these structural conditions, since both are considered normal in mild to moderate forms as we get older.
Herniated Disc Leg Pain Final Thoughts
Sure, herniations can cause leg pain and the associated disturbing neurological tortures. However, most problematic herniations will resolve by themselves, or with appropriate treatment, in a matter of 2 to 8 weeks, on average. Pain which continues for months, or even years, is unlikely to actually be sourced from any herniation, especially when the degree of neurological impingement is questionable.
If your nerve pain in the lower limbs does not get better by itself, or if all the treatments you have tried have not solved your symptomatic expression, please consider the very good possibility that your pain might have nothing at all to do with your bulging disc. The symptoms might be the result of another structural source or may even be the product of a psychosomatic disc pain syndrome.
Your neurologist will help you to make the determination of the actual source of pain. Never leave them out of the diagnostic equation in order to enjoy the best chance for successful symptomatic correlation.
Herniated Disc > Herniated Disc Pain > Herniated Disc Leg Pain





