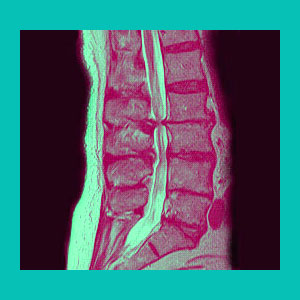
Lumbar herniated disc spinal stenosis is one of the possible consequences of a large and problematic central or paramedial disc protrusion in the lower back. Spinal stenosis is often diagnosed in patients with mildly narrowed spinal canals, which is an iatrogenic mistake. This creates fear and panic in patients with obviously asymptomatic versions of the condition.It is wise for doctors to only diagnose stenosis as the source of pain in patients with obvious central neurological impairments and compressive neuropathy conditions.
This essay explores how lumbar herniations can cause or contribute to decreased patency of the central vertebral canal, also known as spinal stenosis. If your doctor has informed you that you are suffering from lumbar herniated disc spinal stenosis, then this discussion is a Must Read for you.
Lumbar Herniated Disc Spinal Stenosis Causes
Spinal stenosis in the lower back is extremely common, especially as patients age. There are many possible reasons for stenosis to exist, but nearly all factor into the usual and expected aging processes which affect people universally.
Stenotic changes may be a result of bone spurs, also called osteophytes, which build up and limit the space in the spinal canal. Stenosis can also come about due to vertebral misalignment, such as in the case of anterolisthesis or retrolisthesis. Atypical spinal curvatures can play a role in the formation of lumbar stenosis, with scoliosis, hyperlordosis and hypolordosis all being contributory in cases of significant anatomical abnormality.
Some patients are born with a congenitally narrowed central canal, which can be further decreased in patency due to any of the above factors.
However, disc pathologies are the most common stenotic contributor in the lumbar spine, since, after all, they are the most prevalent of all irregular structural conditions in the human vertebral column. It is true that it is extremely rare for a disc herniation to cause a symptomatic version spinal stenosis all by itself.
When combined with ligamentum flavum inflammation or any of the above listed contributors, true and significant canal impingement might be enacted by an intervertebral protrusion.
Lumbar Bulging Disc-Related Spinal Stenosis
In the lumbar spine, the spinal cord breaks into the various structures of the cauda equina somewhere between level T12 and level L3. Most cases of spinal stenosis in the lumbar spine do not have the potential to press on the spinal cord itself, but instead may impinge on one or more of the nerve roots which constitute the cauda equina.Regardless of the possible neurological structures which may or may not be compressed, the following diagnostic process should always be performed:
MRI or CT scan will provide a good visual representation of the lumbar anatomy. This will detail disc abnormalities and other structural pathologies which may be involved in the symptomatic expression.
However, diagnostic imaging will never provide a definitive diagnosis. In order to achieve this, the patient should always undergo neurological correlation and nerve conduction testing, as well as a complete physical exam. These additional steps will assist in preventing misdiagnosis, which is one of the main reasons for herniated disc treatment to fail.
Lumbar Herniated Disc Spinal Stenosis Concerns
Spinal stenosis can be difficult to diagnose, since it can exist anywhere in the backbone and enact symptoms at any location below the affected level.
I see many patients whose pain was blamed on spinal stenosis or foraminal stenosis in the lumbar region, while all along the symptoms in the legs and lower back came about from advanced spinal stenosis in the neck. This occurs often, so be warned.
Additionally, many cases of mild to moderate stenosis are not problematic and are mistakenly named as the painful causation, when all along some other structural or nonstructural causation remains undiscovered, and subsequently, untreated. In essence, never forget that some degree of stenotic change in the lower back is normal and expected. It is rare for these typical stenosis patterns to produce any pain or neurological consequences.
Herniated Disc Spinal Stenosis Overview
The worst cases of spinal stenosis will produce easy to recognize issues, such as balance disorders, muscular weakness, neurological dysfunction, the inability to walk and even severe symptoms, such as cauda equina syndrome.
Stenosis will not usually present the type of pain suffered by the average lumbar dorsopathy sufferer, which obviously exists in the postural muscles of the lower back, buttocks and sometimes the legs.
If you have been diagnosed with lumbar spinal stenosis due to a herniated disc, the incidence of misdiagnosis is greater than those patients diagnosed with arthritic stenosis. Herniated discs most often produce a mass effect on the thecal sac and nothing more. This is just a fancy way to say that the herniation is touching the protective membrane which surrounds the spinal nerve tissues. This is virtually always a completely asymptomatic condition.
Herniated Disc > Herniated Disc in the Lower Back > Lumbar Herniated Disc Spinal Stenosis





