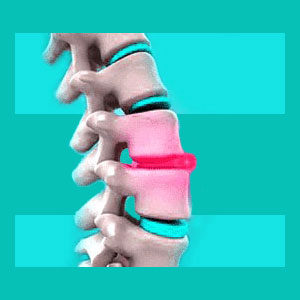
Spinal disc inflammation describes an abnormal swelling of an intervertebral structure. Inflamed discs can occur from discal infection, but herniation is not considered a classic inflammatory process. Many diagnosticians report finding discal inflammation when an intervertebral structure is imaged and seen to be bulging, herniated or ruptured. This is an incorrect conclusion, since inflammation describes a specific type of anatomical reaction to infection or disease, not a simple structural change that occurs due acute trauma or degeneration.
True discal inflammation can occur due to rare contamination of the intervertebral structure itself, often diagnosed as discitis. However, other pathologies that cause the disc to change shape in response to stress or age are certainly not inflammatory processes and should never be diagnosed as such.
This essay examines actual and incorrectly identified intervertebral spinal disc inflammation and the subsequent illogical justification for using a wide range of anti-inflammatory drugs during treatment.
[contentblock id=1]
Spinal Disc Inflammation Explained
Inflammation describes an anatomical reaction to infection, injury or irritation wherein the circulatory structures of the localized anatomy increase heat, fluid retention, pain stimulation and rigidity of tissues that have been traumatized. This process is extremely temporary and protective in design and execution.
In true cases of intervertebral swelling, the only logical cause is discal contamination by an infectious agent. This is most often seen in children, people with compromised immune systems, intravenous drug users and those who endured certain varieties of spinal surgeries and suffered unfortunate postoperative complications.
Since the spinal discs are not visible externally, the inflammatory response can only be seen via certain types of diagnostic imaging studies. Typically, patient history and symptomology will be the likely factors that lead doctors towards performing these tests when they suspect discal infection as the source of pain and related expressions. However, even in cases of true disc infection, the inflammatory process can be quite different than swelling expressed elsewhere in the body, since discs do not have internal blood supplies or nerves, making them unable to express many of the common signs of typical inflammation.
[contentblock id=20]
Misdiagnosed Discal Inflammation
Many doctors and chiropractors will diagnose a bulging or herniated disc as being inflamed. This is incorrect and misleading. Intervertebral herniation is not an inflammatory process. It is not a reaction to infection or a means of temporarily stabilizing an acute trauma within the disc structure.
Instead, intervertebral bulging and herniation simply describe scenarios in which the interior nucleus of the disc applies force to a weakened annulus fibrosus, causing the structural defect. This is not an inflammatory response at all, but instead, a mechanical breakdown caused by age or injury-related stress. Describing a herniated disc as being inflamed is illogical and incorrect.
Furthermore, even when the disc itself is not deemed to be inflamed, the surrounding musculature is often implicated to be affected by an inflammatory process. Once again, this is truly illogical from a diagnostic viewpoint, since there is no clinical evidence of inflammation. There may be pain and stiffness, or even innervation problems, but these factors are not caused by the traditional fluid-accumulation common to true inflammatory events.
The logic in all these facts is easily proven since inflammation is an extremely transitory happening in a localized area. It will not likely continue for long and certainly will not take place for the years or decades that many back and neck pain patients suffer with their chronic disc-related symptoms.
Spinal Disc Inflammation Treatment
Pharmaceutical interventions represent the most common and widely used therapies for herniated discs, as well as for back and neck pain syndromes of all varieties and theorized causations. Therefore, a diverse selection of anti-inflammatory drugs have found a home in the treatment of all manner of dorsalgia conditions, despite there being no inflammation present to justify their application.
Steroidal drugs can be taken orally or injected locally. In fact cortico-steroids, such as cortisone, are some of the most widely used substances in all manner of back pain injection therapies.
[contentblock id=18]
Nonsteroidal anti-inflammatory drugs, also called NSAIDs, are usually taken orally and represent some of the most common prescription medications for chronic pain sufferers. These drugs work great to reduce traditional, actual inflammation and are used successfully in many acute injury and infectious process treatment routines. However, when prescribed for years at a time for a dorsalgia condition, where typical spinal disc inflammation is clearly absent, the use of these substances falls nothing short of iatrogenic error.
All these substances are dangerous and can cause a variety of nasty effects, regardless of how they are utilized. Despite these risks and the lack of indications for their use, anti-inflammatory agents continue to be mainstays of the pharmaceutical care sector even in this “enlightened age” of medical treatment.
Patients love these drugs, since virtually all of them have analgesic properties as well as anti-swelling agents, so they do provide some degree of relief for most conditions. However, doctors would be better served using pure analgesic drugs with fewer serious side effects than these combined-use products that are known to cause anatomical harm, particularly when employed long-term.
If you are currently using a steroidal or nonsteroidal anti-inflammatory agent orally, or through injection therapy, it might be wise to discuss the reason for the prescription with your doctor and investigate alternative and more logical options.
[contentblock id=2]



