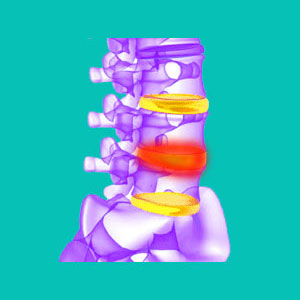
A swollen spinal disc is a misleading diagnosis, since intervertebral discs do not suffer true versions of inflammation when they bulge or herniate. Swelling denotes the abnormal accumulation and retention of moisture, otherwise known as inflammation. Other typical signs of inflammatory swelling include redness, heat generation and pain, none of which are symptoms that are linked to most cases of intervertebral bulging.
Swelling is a natural process that is caused in reaction to trauma, infection or disease. While herniated discs can also be caused by injury, the way that they react to the stress of trauma is very different than most other bodily tissues. Therefore, swelling is not an accurate term to describe the structural changes in any bulging disc, regardless of the cause of these changes.
Despite the logic of these facts, we continue to receive many letters from readers that state a diagnosis of a swollen spinal disc was received from a doctor or chiropractor, leading the patient to seek advice on the best disc pain treatment. While we cover treatment elsewhere in this comprehensive online web resource, we have decided to devote this dialog to the subject of intervertebral disc swelling, since it seems to be greatly misunderstood by so many affected patients.
[contentblock id=1]
Why Are They Called Swollen Spinal Discs?
Most diagnosticians will not utilize the term “swelling” to describe any change in intervertebral structure, unless the condition involves some true inflammatory process, such as that occasionally demonstrated during discal infection, also known as discitis.
However, some diagnosticians will use laymen’s terms, such as “swollen” or “swelling” to describe intervertebral bulging or herniation. These are incorrect uses of these descriptive terminologies that mislead patients into associating structural disc change with that of a true inflammatory process.
We see a continuing trend towards infantilizing patients and speaking to them in terminologies that do not accurately reflect the condition being described. This means that patients are not given medical diagnoses, but instead are given “watered-down” and “simplified” versions of actual diagnostic findings in order to facilitate easier comprehension of the data collected during evaluation. This is usually done to save doctors the time it takes to explain the more technical aspects of proper diagnostic findings and conclusions. Instead, it is easier to use words that the patient can easily relate to, such as “swelling”, even though these words do not in any way accurately portray the condition found within the spinal anatomy.
[contentblock id=19]
This “dumbing-down” of the diagnostic process has caused countless misunderstandings and is often cited as causative or contributory towards poor therapy results, based on patients receiving treatments that are not actually indicated for their true condition, but instead targeted towards diagnoses, such as inflammation, that do not reflect the actuality of the disc structure.
Swollen Intervertebral Disc Realities
When a spinal disc bulges or herniates, there is no accumulation or retention of moisture. There is no redness demonstrated or heat generated. There may or may not be pain, but discomfort is certainly not inherent to the herniation process. Instead, the outer disc wall simply changes shape, allowing the interior nucleus to form a focal or diffuse section of asymmetry in the overall disc structure. Imagine a small bump or pocket of jelly pushing outward from the disc wall and you have a pretty accurate laymen’s description of intervertebral bulging or protrusion.
When herniated discs occur, there is no inflammation or swelling. There is merely a structural change that may or may not be permanent. In fact, clinical observation clearly shows that the spinal discs are always changing in shape and symmetry, in response to stress, age, the normal daily cycle of water retention and other factors. Herniation is just one more of these normal changes that occur in many spinal discs.
We have already detailed the causes of herniated discs and demonstrated that most of the disc bulges occur due to completely universal age and activity-related circumstances. Therefore, by definition, herniated discs should be considered normal; not atypical. This idea is receiving increased acceptance among doctors each and every year, since the evidence of the virtual universality of intervertebral abnormalities is indisputable. Herniated discs are no longer considered inherently pathological and most have been proven to be coincidental to any pain suffered. The same can not be said for inflammation, which is always a painful process that sends an anatomical alert that something is wrong to warrant such an obvious bodily reaction.
Swollen Spinal Disc Conclusions
We have been pleading with diagnosticians for a decade already to stop using laymen’s terminology to inaccurately describe specific medical conditions, such as intervertebral bulging or protrusion. “Swollen” and “inflamed” do not portray the reality of spinal disc changes in virtually every case, with the few exceptions of extreme discitis mentioned above.
[contentblock id=18]
Patients must stop associating their vision of inflammation with what is truly occurring in their spines, in the case of herniated discs. There is no swelling. There is merely a normal breakdown of structural integrity, leading to a change in symmetry and a possible loss of interior nucleus pulposus material through an annular tear or disc rupture.
Patients must cease looking for treatments that target inflammation, since their discs are not inflamed. This includes the many complimentary care practices that are geared towards reducing swelling and the plethora of dietary and pharmaceutical products that have anti-inflammatory properties.
We further recommend that doctors discontinue the prescribing of anti-inflammatory agents for virtually all cases of back or neck pain, since in 99.9% of patients, there is no inflammatory process demonstrated. Analgesic medications are fine, as long as patients understand the many risks, but anti-swelling chemicals are not indicated for herniated discs in any way.
We hope that this essay helps to clarify what has become a real problem in the understanding of one of the most common of all dorsalgia diagnoses: the herniated disc. Sure, the disc may be bulging, but it is not truly an inflamed or swollen spinal disc and should never be treated as such.
[contentblock id=2]



