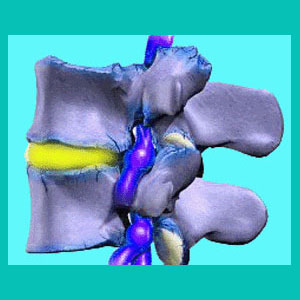
A thoracic herniated disc pinched nerve is truly a rare occurrence and is not generally found in many patients, unless they have been subjected to severe trauma, such as a car accident or significant fall. The thoracic spine is not an area subject to normal degenerative processes, since it is built for support and stability, not flexibility. Being that it does not need to flex too much or too often, the thoracic spine seldom suffers degenerative disc disease and therefore, most herniated discs are sourced through spontaneous traumatic injury.
Remember that a bulging disc can close off much of the foraminal space on the inside or outside of the opening without influencing the nerve at all. When the nerve is touched or displaced, symptoms are not bound to occur, but will almost certainly present themselves when the nerve root is actually pressured forcefully by the offending disc material.
This dissertation explores the occurrence of pinched nerve conditions as a result of intervertebral bulging or rupture.
[contentblock id=1]
Thoracic Herniated Disc Pinched Nerve Facts
Pinched nerves feature the same characteristics, wherever they may occur in spine. Although pinched nerves in the middle back are rare, they will still demonstrate identical symptomology as other spinal locations, such as compressive neuropathies in the lumbar spine or cervical spine.
Nerve compression occurs when a herniated disc bulges or ruptures into the neuroforaminal space, sealing it off and applying pressure to the spinal nerve root. This is well documented to produce total objective numbness and weakness over time, but not the often misdiagnosed symptoms of lasting pain, enduring tingling and subjective chronic numbness and weakness in most instances.
Lasting pain may indicate incomplete compression or another root process at play to better explain the symptoms.
[contentblock id=15]
Thoracic Pinched Nerve Details
The thoracic spine is the least common area to suffer both degenerative disc disease and herniated discs. The middle back is strong, stable and is rarely the location of chronic back pain syndromes. Most chronic discomfort experienced in the middle back is ischemic or due to another anatomical source, not some possibly coincidentally diagnosed disc issue.
When degenerative disc pathologies do exist, they reside most commonly at the cervicothoracic juncture or within the first few thoracic intervertebral levels. Sometimes, they may also occur at the thoracolumbar juncture or the last few thoracic levels.
However, patients who have suffered a tremendous accident or injury to the middle back may indeed suffer physically-induced pain due to general trauma or even from various other disc pain processes, like spinal stenosis or chemical radiculitis.
Thoracic Herniated Disc Pinched Nerve Link
While pinched nerves in the middle back are rare, they can occur and may need drastic or even surgical treatment. The good news is that correctly identified and diagnosed nerve compression issues anywhere in the spine generally resolve with indicated therapy.
For patients who do not get better, the most logical and common explanation is simple mistaken diagnosis of the actual source of pain. This is an epidemic problem in the healthcare system and is particularly prevalent in the back pain industry. Statistics show that all manner of disc pathologies are the most common of all misdiagnosed back and neck pain concerns.
[contentblock id=2]
Herniated Disc > Herniated Disc in the Upper Back > Thoracic Herniated Disc Pinched Nerve



