A torn spinal disc can be a scary diagnosis for any affected patient to receive from their physician. It is important to understand the anatomy of an intervertebral disc in order to realize that most minor annular tears in the outer disc wall are commonplace and very rarely symptomatic. Actually, since a disc has no blood supply or nerve endings, a torn annulus fibrosus is seldom problematic, but may lead to chemical radiculitis concerns in some patients.
This essay will look at damaged spinal discs which feature holes in the outer disc wall structures. We will look at why these holes occur and their potential effects on the patient.
What is a Torn Spinal Disc?
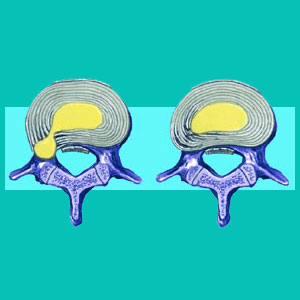
An intervertebral disc is made up of 2 sections, the annulus fibrous and the nucleus pulposus. In the cases of a disc tear, the hole appears in the outer disc wall, the annulus, and may facilitate leaking of some or all of the nucleus pulposus. While it sounds really bad to have a hole in a disc wall, it is actually a rather common event. Many of these conditions exist for years or even decades without being discovered, since they cause no pain or health risks whatsoever.
The most common locations for annular tears are in the lumbar and cervical spinal regions. This is no surprise, since these are the areas which suffer the most intervertebral deterioration and also demonstrate the highest incidence of traumatic injury.
Both degenerative disc disease and injury can cause holes to form in the outer disc annulus, although degenerative cases are statistically far less symptomatic than ruptures enacted by trauma.
Consequences of a Torn Intervertebral Disc
Many small tears do not change the disc structure at all. They are simply there, without causing any real concerns. Large holes or tears can allow the nucleus to slowly or suddenly leak from the disc structure.
There are proteins in the nucleus which are theorized to be irritating to neurological tissue in some patients. Not all ruptured discs will cause chemical radiculitis, but the symptomatic expression is possible for some patients. In these cases, a series of epidural injections is typically the best treatment, since the irritating proteins can be neutralized and flushed away rather easily in most cases.
If not treated, the body will eventually absorb the leaked disc material anyway or it may calcify in other instances. If it does calcify on or around nerve tissue, true nerve or spinal cord compression has a better chance of developing, possibly necessitating the application of a surgical intervention to free up the neurological tissue.
Torn Spinal Disc Changes
Annular tears are often diagnosed on MRI imaging, since this advanced form of testing can clearly visualize even the smallest details of the spinal anatomy. Many patients fear that they will require surgery to correct a torn disc, but this is seldom the case. In fact, surgery is rarely advised, since it will not likely do anything to correct pain, whether it is actually related to the disc, or is coincidental, as is the case in some diagnosed patients.
Some patients ask if annular tears can heal by themselves and the answer is yes and no. They may heal or simply never become symptomatic, but they may not. Some annular tears create accelerated degeneration of the disc structure, but this is normal and not usually a cause for alarm.
Remember, the overwhelming majority of disc issues are not painful or dangerous. Discs may be blamed for causing the majority of back, neck and sciatica pain, but there is little, if any, scientific evidence actually linking disc abnormalities and chronic pain in the majority of diagnosed cases. The exceptions to this rule exist when the disc demonstrates a definitive pathological process, such as the aforementioned compression of a nerve or the spinal cord.





