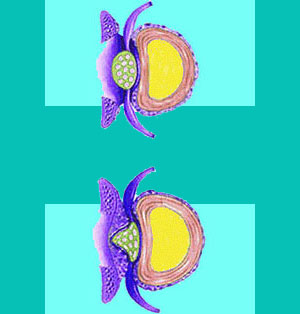
Spinal stenosis is a potentially serious condition in which the central vertebral canal is narrowed by one or more factors, potentially compressing the spinal cord or cauda equina. Stenosis is a grossly over-diagnosed occurence, since mild to moderate asymptomatic versions of the condition are actually a normal part of the aging process for most patients. In many scenarios, the canal can be minimally or moderately decreased in size without any symptoms occurring. However, if true neurological constriction does occur, there are few back and neck pain syndromes which can cause such severe and diverse tortures throughout the anatomy.
It must be noted that stenosis that is caused by spinal disc herniations may resolve all by itself. Herniated discs can be transitory spinal abnormalities and when they narrow the canal space, the result is not always permanent stenosis. Many of these disc-enacted stenotic changes only partially close off the central canal and many will resolve, even without treatment.
Herniations will have the best chance of truly causing symptomatic stenosis when they exist in combination with other spinal abnormalities at the same level. Arthritic change, ligamentous inflammation or a congenitally narrow canal can all increase the likelihood of symptomatic stenosis happening with a central disc prolapse condition.
This article will detail various forms and locations for spinal stenosis to occur in relation to a herniated disc.
What is Spinal Stenosis?
Stenosis is a term which describes a narrowing of an anatomical opening. In the case of the backbone, this condition refers to a reduction in the size of the spinal canal. The central canal is the sheath which surrounds the spinal cord and spinal nerves. If the spinal canal narrows, it can encroach on the actual cord or nerve roots, potentially causing serious neurological symptoms.
As we age, normal degenerative changes in the spine can create a stenosis condition, typically in the neck and lower back. Osteoarthritis changes the structure of the vertebrae, thereby often effectively reducing the size of the spinal canal. These changes usually do not produce any discomfort, but they might create minor aches and pains in some patients.
Highly symptomatic stenosis is rare, but can be a huge problem if the condition becomes extreme. Cauda equina syndrome can result from advanced spinal stenosis in the lumbar spine. Spinal stenosis may be sourced from a herniated disc or other structural issue. Learn about all the causes and symptoms of stenosis, as well as treatment choices from Spinal-Stenosis-Treatment.Org.
Causes of Spinal Canal Stenosis
As previously mentioned, the normal aging process enacts minor stenosis in many individuals as they reach old age. However, this non-painful or mildly uncomfortable condition should not be confused with advanced cases of spinal canal narrowing. True, it is stenosis to some degree, but does not warrant treatment or even considerable worry. Causes of the more serious stenosis condition range greatly:
Degenerative disc disease and the various forms of spinal arthritis certainly can cause significant stenosis in rare circumstances.
A traumatic herniated disc injury might bulge the disc core directly into the spinal cord or cauda equina, causing a sudden acute stenosis concern.
Spondylolisthesis can also cause stenosis and the degenerative form of the condition can cause spinal canal narrowing gradually or abruptly.
Learn more about a herniated disc causing stenosis.
Spinal Stenosis Symptoms
Severe deep neck or back pain is the most universal symptom of real stenosis. Neurological issues, such as tingling, weakness and numbness might coexist with pain or even instead of pain. The most extreme examples of stenotic change may elicit incontinence and the inability to stand. Often times, standing will bring on symptoms and sitting will help to relieve the pain, especially when the stenosis exists in the lower back.
Severe cases of stenosis can create potential medical emergencies, such as cauda equina syndrome or nerve compression leading to systemic failure of an autonomic process. These circumstances can produce dire results and must be handled by a qualified medical professional immediately.
Minor stenosis pain is nothing to be concerned about and is not generally progressive. This form of stenosis might create stiffness, minor arthritic pain and an occasional sharp twinge in the back. This is indeed one of the costs of aging, but if the condition is not obsessed over, most cases will not become problematic.
The nocebo effect of the diagnostic process is key to determining whether or not symptoms will intensify or resolve in some patients. This is why it is so important to learn the facts about the common nature of spinal stenosis and to not allow a doctor to literally scare you into experiencing undue pain.
Help for Spinal Canal Stenosis
Stenosis is a complicated condition to deal with, since so many of us normally develop it as an expected part of getting older. Some of us will not be affected by the physical changes in our spines and never even acknowledge the condition. Others will be diagnosed with stenosis and will have a choice to make.
If these patients subscribe to the theory that stenosis is inherently painful, then they are likely to develop progressively worse symptoms. If the understand the reality of stenosis, they are not likely to suffer, unless the condition progresses to severe degrees of canal impingement.
A few of us will unfortunately be struck down by the most severe forms of this condition, which can cause a health crisis for any affected patient. These poor souls will likely require surgical interventions and might never fully recover.
The variable profile of stenosis sometimes makes it difficult to determine which group you might fall into. My advice is to get more than one opinion on your diagnosis. If therapy is needed, start treatment conservatively and save surgical modalities as a very last resort.
Obviously, if you are among the few with the worst possible form of the condition, all bets are off. You might have to skip directly to a surgical solution and will hopefully be one of those who can truly recover full functionality.





