We have prepared this easy-to-understand herniated disc guide to help patients who are currently affected by back or neck pain that is thought to exist due to intervertebral pathology. Reading through this guide will assist any patient in navigating the confusing diagnostic and treatment processes.
Herniated discs are some of the most common structural back and neck abnormalities and are also typically linked to causing painful symptoms. Of all the dorsalgia topics we cover, herniated discs remain one of the most misunderstood of all subjects.
Worse still, herniated disc-related questions account for the majority of reader inquiries we receive across the many websites of The Cure Back Pain Network. Obviously, the subject is so important that we have devoted this entire web resource to covering it in the greatest detail imaginable.
This herniated disc guide contains an overview of intervertebral herniations. We will examine what they are, why they exist and how they are diagnosed. We will also provide some easy tips on treating damaged spinal discs for best results.
Herniated Disc Guide / What Are Herniated Discs?
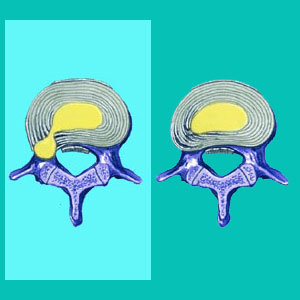
Spinal disc herniations describe a condition wherein a typical intervertebral spacer loses its normal symmetrical shape and develops a bulge of nucleus material that swells against the outer disc wall. Typically, this outer wall, called the annulus fibrosus, contains the nucleus within the center of the disc structure. However, in a herniation, some of this soft center pressurizes the outer wall and the disc develops an asymmetrical area of swelling.
Herniations come in many forms and severities, ranging from broad-based bulges to focal protrusions to cases where the outer disc wall becomes compromised and allows the interior nucleus to leak out of the contained disc mass. These annular tears can result in small amounts of nucleus escaping over time or might involve spontaneous disc rupture that allows the entire nucleus to egress from the annulus, sometimes with devastating consequences.
Terminology for herniated discs ranges greatly and is not universally applied. Doctors often use their own arbitrary descriptive nomenclature and this can be incredibly confusing for the patient, who is never quite sure how bad their disc issue truly is.
For more information on what constitutes an intervertebral herniation, we highly recommend reading through our comprehensive resource section titled: What is a herniated disc?
Herniated Disc Guide / Causes of Intervertebral Herniation
The vast majority of patients who contact us clearly do not know that herniated discs do not have to be caused by any specific injurious event. Many have been misinformed by their doctors that herniations must have occurred due to some known recent trauma, often because pain begins at some point after the “injury” occurred.
Research clearly shows that many herniations exist in the spinal anatomy, yet cause no pain whatsoever. In fact, most herniations are considered completely asymptomatic, even when coincidental back or neck pain exists, since there is no link between the symptoms and the disc deterioration. So, where do herniations actually come from? Well, there are many possibilities that may or may not answer this question for any given patient:
Herniated discs can indeed be caused by injury. These are called trauma-induced herniations, but many are actually caused through a combination of injurious stress and previous degeneration acting together to enact the change in structure.
Herniated discs can also come about through normal or accelerated spinal deterioration. Several normal spinal aging processes assist herniations to form, including disc desiccation. It should be noted that degeneration-related herniations are usually among the least symptomatic varieties.
Herniations can occur due to congenital, genetic or developed traits. These may or may not be identifiable. If not, the herniations will usually be deemed idiopathic, since it occurs without particular and definable explanation.
Full details on the many possible contributors to intervertebral bulging can be found in our herniated disc causes resource section.
Herniated Disc Guide / Symptoms of Intervertebral Herniation
Symptomatic expressions of herniated discs range greatly. Most disc bulges do not generate symptoms and probably never will. Some herniations source acute symptoms for a time and then resolve, without any treatment needed at all. Other herniations produce the types of symptoms that compose our collective nightmares; chronic and intractable pain, often combined with neurological dysfunction.
Ironically, the severity of the herniation has little to do with the degree of symptomology in virtually every case. We have seen truly horrific intervertebral herniations where the patient had no pain and did not even realize they had anything structurally “wrong” with their spinal column. These herniations are often located during routine imaging studies for unrelated conditions.
We have also seen minor herniations that happen to occur in specific ways that influence the spinal neurological functionality to a terrible degree. Some patients are disabled by relatively minor and seemingly inconsequential disc bulges.
It must be mentioned that herniated discs feel no pain themselves. The disc has no interior nerve endings or blood supply. It is little more than a fibro-cartilage shell with a soft jelly center. The reason why herniations might produce symptoms is when they influence the surrounding spinal nerves in some manner, typically through compression or chemical irritation.
For complete coverage of the possible symptomatic expressions, please read through our in-depth section titled symptoms of a herniated disc.
Herniated Disc Guidance / Diagnosis of Herniated Discs
Positive diagnosis of any intervertebral pathology or abnormality can not be made without the benefit of advanced diagnostic imaging. This means application of CT or MRI technology.
X-ray technology can determine that a disc abnormality might exist, but rarely can identify the degree or nature of the structural change, since it does not image these soft tissues, unless one happens to calcify into bone. Then, even antiquated x-ray will paint a relatively vivid picture of the intervertebral level in question.
There is no other way to accurately diagnose any disc pathology. There is no test, such as the commonly used straight-leg raising test, which can diagnose a bulging disc. There is also no set of symptoms that will positively identify a herniation.
Doctors will use the symptomatic complaint and may employ some non-imaging tests to narrow down the diagnostic possibilities before ordering a CT or MRI. However, any care provider who makes the actual diagnosis without the benefit of imaging should be avoided. These doctors are speculating on your health, which is unethical, unprofessional and virtually illegal. Find a new caregiver for best results.
To learn more about what exactly qualifies a herniation and how they are identified, please peruse our herniated disc diagnosis section.
Herniated Disc Guide / Treatment for Herniated Discs
Herniated disc treatment is by far the most complicated topic for patients to understand. This is due to all the many factors we have described above, as well as many others listed below.
Many discs do not need any treatment, since they are not the actual origin of pain. They might have been mistakenly identified as the source, but they remain innocent. We see this sad occurrence each and every day. This is the main reason why so many treatments fail to deliver satisfying outcomes. After all, the therapy techniques are not being used to resolve the true causation of symptoms in the back or neck.
For discs that do require care, time alone may be the best path toward relief. Many herniations will get better without any professional care. However, the timeline is uncertain and many patients simply get tired of living in pain while they wait.
Some pathological discs might enjoy some degree of improvement, or even total healing, from conservative care, such as physical therapy, typical chiropractic or other hands-on modality. These do not represent the rule, but instead, the gross exceptions.
Spinal decompression is a nonsurgical moderate therapy approach that is highly effective for resolving some herniations. Although expensive, the method is proven to work well for many different intervertebral diagnoses and allows the patient to avoid surgical intervention.
Minimally invasive approaches to care might be useful for many types of herniations, as well. Injection-based treatments, such as flushing epidurals, might be effective for relieving chemical irritation of nerve fibers. However, anesthetic and steroid-based epidurals will rarely do anything for contained herniations, except possibly provide temporary analgesia.
Less invasive surgical practices, such as IDET and nucleoplasty, are also good considerations for certain types of contained herniations.
Full surgical endeavors, such as discectomy, laminectomy, disc replacement and spinal fusion should be avoided whenever possible, but still offer possible solutions for patients without any other options. It must be noted that disc-related procedures demonstrate the very worst results in the dorsalgia surgery arena over timelines of 7 years. Therefore, patients are sternly warned to save true surgical correction as a final selection, once all other possibilities have proven fruitless.
For full coverage of these crucial therapy topics, please refer to our herniated disc treatment and herniated disc surgery sections. We hope that you have enjoyed this herniated disc guide and that it has helped to clarify the facts of the condition for you.
Herniated Disc > Herniated Disc Story > Herniated Disc Guide






