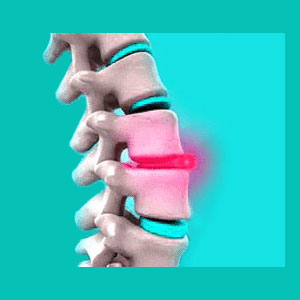
A broad based herniated disc may also go by many other names including diffuse herniated disc, diffuse disc bulge, broad based disc bulge, broad based disc protrusion, broad based disc herniation or broad based prolapsed disc. This type of herniation, like all other varieties, describes a condition in which the nucleus pulposus bulges or ruptures through the outer annulus fibrosus. To put this is simple layman’s terms, the soft moisture-filled center of the spinal disc bulges into a pocket in the outer disc wall or may actually break through the outer wall, typically called a ruptured disc.
This educational essay focuses on explaining broad based intervertebral bulges and extrusions in the spinal anatomy.
Broad Based Herniated Disc Nomenclature
The addition of the term broad-based to any herniated disc diagnosis simply refers to the proportional size of the actual bulge or herniation. When the size of the herniation is 25% to 50% of the total disc circumference, the disc pathology is described as being broad based. When the degree of bulge is less than 25%, the condition is described as being a focal herniated disc. Sometimes a broad based herniation is represented on a circular map, in which case, the herniated portion is 90 to 180 degrees of the total 360.
In many cases, the diagnostic term diffuse is substituted for broad based, but many care providers also use the term diffuse to mean general widespread or symmetrical bulging, as well. The terminology used here is really quite irrelevant to patients, but these names often provide some degree of confusion on MRI and CT scan reports, so it is always a good idea to understand what they mean, at least in a very basic sense.
Broad Based Bulging Disc Prognosis
Broad based bulging discs are not any inherently worse than focal protrusions. Most broad based disc protrusions are not symptomatic or harmful in any way, although some may enact pain and possible related symptoms if they affect a neurological structure.
Broad based central herniated discs are often reported to impinge on the thecal sac, which basically amounts to nothing. These herniations seldom provide any cause for alarm, although they often act as back pain scapegoats. Central herniated discs also may compress the actual spinal cord in some scenarios, enacting spinal stenosis and possibly requiring treatment.
Broad based posterolateral herniated discs bulge towards the sides of the spinal canal, often entering what is known as the lateral recess. This is simply a space on the sides of the central canal. In some circumstances, lateral herniations may cause foraminal stenosis, which is defined as a narrowing of the space through which the spinal nerve roots pass.
In very rare instances, the herniation may actually contact or compress a spinal nerve root, potentially causing neurological effects in the area of the body served by the constricted nerve tissue.
Broad Based Herniated Disc Help
Many diffuse herniations are found in diagnostic imaging studies, regardless of whether the patient has back pain or not. I always advise patients to learn all the facts about herniated discs before seeking any type of treatment and also getting at least 2 to 3 different opinions from a variety of care providers, including an orthopedist and a neurologist.
It is easy to get caught up in: “I have a (insert diagnosis here)”, without really understanding what it all means. This mindset is not helpful if you do not understand what the diagnosis actually is and how it corresponds (or doesn’t, as the case often is) to the actual symptoms experienced.
Herniated Disc > What is a Herniated Disc > Broad Based Herniated Disc




