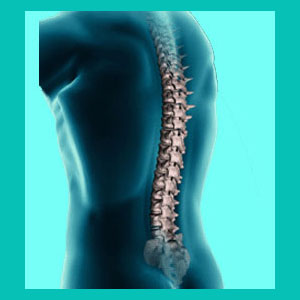
A herniated disc in the middle back occurs less often than a disc injury in the lower back or neck. The middle back is built for support and structure, providing needed protection for our internal organs and the very frame work for our skeletal system. The mid back is not called on to perform the same frequency of vertebral motions as the other spinal areas and for this reason is less susceptible to both traumatic injury and degenerative changes.
When a herniation is diagnosed in the middle back, without known traumatic causation, the condition is often enigmatic. Most mid back disc pathologies are enacted by damaging accidents and injuries, since the usual spinal aging processes are rarely found in the middle thoracic levels to any significant degree.
This dialog focuses on middle back intervertebral abnormalities adn their consequences on the surrounding spinal anatomy.
Herniated Disc in the Middle Back Causes
The mid back does not have to bend or flex often at the intervertebral joints, making it less prone to developing the symptoms of common spinal degeneration, including spinal osteoarthritis and degenerative disc disease. This fact makes the incidence of degenerative herniated discs in the mid back far less common.
Herniations in the middle back which are not linked to trauma are usually theorized to exist due to other structural issues presented by particular patients. These may include kyphotic changes to the upper back or side-to-side spinal curvatures in the mid back. Only a minority of thoracic bulges will be deemed truly caused through usual spinal deterioration.
The middle back is still able to be injured by significant trauma and might suffer a disc herniation in such circumstances as an automobile accident, a sporting injury or a fall.
Thoracic herniated discs are the rarest of all disc problems and also typically resolve the best.
Symptoms of a Mid Back Herniated Disc
As with any other disc herniation, symptoms for thoracic bulging discs include localized and radiating pain. Some patients might experience tingling, numbness or weakness in the shoulders, base of the skull, arms or hands. This is a sure sign of nerve involvement, but does not always mean the herniated disc is the cause.
Oxygen deprivation is a common back pain syndrome which is often overlooked when a herniated disc diagnosis is made.
Thoracic outlet syndrome is another possible source of neurological symptoms, even though it is enacted by the upper back muscles and not by any coincidental spinal abnormalities.
Although acute disc pain might be severe, especially if there was considerable trauma to various spinal tissues, the discomfort is typically short lived. Long-term pain which is blamed on a herniated disc is typically misdiagnosed and is virtually always the result of a structural issue in the neck or a mindbody ischemia condition instead.
Herniated Disc in the Middle Back Circumstances
Remember, the discs in the middle back are the strongest and least likely to be injured in the entire body. Additionally, they heal the fastest and the best. Unrelenting chronic back pain is extremely unlikely from a thoracic disc injury, unless the trauma has literally destroyed the integrity of the spine. If you have been suffering for a long time and have not received any relief from a variety of appropriate herniated disc treatments, you must consider the idea that your pain might have been misdiagnosed. This occurs far more often than you might think and is the #1 reason why so many disc patients never truly recover from their pain.
It makes sense… How can therapy work to resolve pain when it is directed at a mistakenly identified causation? The simple and unfortunate answer: It can’t.
Herniated Disc > Herniated Disc in the Upper Back > Herniated Disc in the Middle Back




