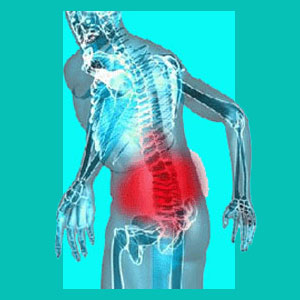
Having a herniated disc problem urinating is a rare but potentially very serious complication of neurological involvement due to a bulging or ruptured disc structure. Urinary concerns can take several forms, but should always be checked out by a qualified care provider, to rule out any very severe neurological disorders or other potentially catastrophic conditions which may leave permanent damage. To this end, I usually recommend a combination diagnostic evaluation from both a neurologist and a urologist.
This article will focus on the 2 most typical urinary concerns suffered by herniated disc patients: incontinence and the inability to urinate. This essay will also look at alternative explanations for these symptoms in cases where the herniation is deemed to be coincidental to the urinary problems.
Herniated Disc Problem Urinating / Can’t Go
Many times the inability to urinate is linked to a psychosomatic disc pain syndrome which acts as a back pain substitute symptom. The inability to urinate is often linked to repressed emotional issues, social phobias and may even be an unforeseen side effect of some drugs.
There are also possible anatomical reasons why it may be difficult to pass urine, but these are not as likely to be related to a herniated disc condition, unless there is definitive nerve compression of the appropriate neurological structures. Typically, patients with neurological involvement which causes urinary issues from herniations can not stop themselves from urinating.
In cases of chronic inability to urinate when no definitive structural reason is discovered, I suggest knowledge therapy as a possible alternative treatment option. Just be sure that your urologist has checked out the anatomical tissues and cleared you of all possible contributing structural issues first.
Herniated Disc Urination / Can’t Stop
Some herniated disc patients suffer urinary incontinence a a direct result of their spinal issues, while others experience similar symptoms from some other anatomical or psychoemotional causation.
True nerve compression can enact cauda equina syndrome, which may cause incontinence and other serious symptoms. Spinal stenosis virtually anywhere in the vertebral column can do the same in extreme cases. These types of symptomatic expressions should always be treated immediately by a qualified emergency medical team.
If no definitive structural reasons for the urinary issues are discovered, I once again suggest knowledge therapy as a different approach to treatment, since the source of the problem may be of mindbody origin. This is especially true if the incontinence occurs overnight or only in specific situations, such as in social settings.
Herniated Disc Problem Urinating Help
Any urinary problems should always be reported to your doctor. Concerns which involve the inability to control passing urine may be medical emergencies and should be reported to your local hospital or trauma center immediately.
Cauda equina syndrome can occur from herniated discs in the lower back. Herniated discs which compress the cauda equina nerves can prevent neurological impulses from reaching the structures which allow normal urination. Additionally, central spinal stenosis in the neck or back can also cause urinary incontinence.
Do not wait if these symptoms occur spontaneously. Get to a doctor right away to prevent any permanent nerve damage from diminishing your future quality of life.
Herniated Disc > Herniated Disc Symptoms > Herniated Disc Problem Urinating




