A pinched nerve from a herniated disc is one of the most common diagnostic explanations for chronic back pain in virtually every area of the spine. However, as in most diagnostic speculations, the pinched nerve theory can be full of ideological holes and often just does not make sense when compared to the actual symptoms demonstrated by the majority of diagnosed patients. Although pinched nerves can and do exist, the likelihood of a herniated disc enacting one for any length of time is not nearly as common as some doctors and patients might think.
This discussion will profile pinched nerves and how they truly occur. We will examine the role played by herniations in causing compressive neuropathy conditions through foraminal, central and lateral recess stenosis.
Pinched Nerve from a Herniated Disc Theory
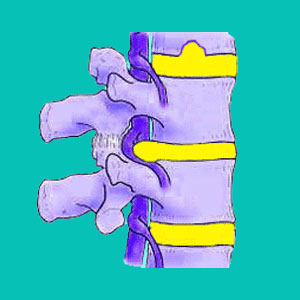
Pinched nerves, when used as a spinal diagnosis, refer to actual anatomical compression of a spinal nerve root structure, most commonly just as it leaves the spinal canal through the neuroforaminal opening. In these cases, the herniated disc is suspected of pressing into the foraminal space, narrowing it and causing a mass effect on the nerve root. While herniations certainly do influence the foraminal spaces, they rarely compress anything or cause any problematic effects.
Research shows that in order for a nerve to suffer compression, virtually the entire foraminal opening would have to be sealed off by the bulging disc, under pressure, which almost never occurs.
Additionally, true ongoing nerve compression creates objective numbness in the affected nerve root, not pain, tingling or subjective numbness commonly demonstrated.
In other instances, the nerve root can be compressed in the lateral recess, before it seeks egress through the foraminal opening. Once again, although this is certainly possible, especially from large focal posterolateral bulges, it is rarely definitively proven in most suspected cases.
Finally, in the middle and lower lumbar spine, central spinal stenosis can compress one or more of the nerve roots which compose the cauda equina. This can have terribly affective neurological consequences when the diagnostic verdict is accurate.
Herniated Disc Nerve Compression
The structural compression theory just does not mesh with most symptomatic expressions. However, the theory of ischemia often makes perfect sense, since oxygen deprivation can certainly causes the variable symptoms typically reported by most herniated disc sufferers. In these cases, the herniation and foraminal stenosis are completely coincidental to the pain and regional ischemia is the true causation.
These cases account for a great number of patient profiles, but are seldom accurately diagnosed, leading to the epidemic of failed back pain treatments so common in the healthcare sector.
Pinched Nerve from a Herniated Disc Considerations
A pinched nerve from a herniated disc is a common diagnosis, but rarely enjoys verifiable evidence to support the conclusion. Some doctors who make the diagnosis do not have any real comprehension of how nerves even work and how compression totally prevents the transmission of the very signals which would create pain.
Meanwhile, doctors use nerve burning and cutting as a treatment, proving that interrupting the flow of nerve energy provides relief, not pain. It is such an idiotic notion in many cases that I have a difficult time understanding how anyone believes the compressive neuropathy diagnosis to begin with.
Then, I remember why: Most patients, such as my former self, do not understand exactly what is going on in their spines and their doctors do not help to clarify the condition at all. Instead, most patients are fed misconceptions and mythologies about the structural model for back pain which have long been proven completely inaccurate.
Descartes is dead and his insistence of separation of the mind from the body is a mistake. The fact remains that a great number of chronic misdiagnosed disc pain cases are a direct result of the mindbody process and not related at all to any anatomical abnormality at all.
Of course, when a pinched nerve diagnosis is made by a neurologist and does benefit from definitive evidence, then treatments will be both appropriate, and most often, successful. Unless this represents your situation, never take a pinched nerve diagnosis for granted as being correct.
Herniated Disc > Herniated Disc Injury > Pinched Nerve from a Herniated Disc





