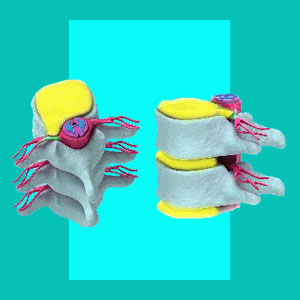
Herniated disc neuroforaminal stenosis is a diagnosis that entails a narrowing of the foraminal spaces, through which the spinal nerve roots egress the vertebral column. Foraminal stenosis occurs in our spines as a normal part of the aging process. The neuroforamen can be narrowed by bulging discs, osteoarthritic-enacted bone spurs and other factors, but this does not mean that symptoms will inherently be produced. In fact, most narrowed foramen are completely normal and asymptomatic occurrences in the lumbar and cervical spinal zones.
This commentary examines how foraminal stenosis occurs due to intervertebral disc changes and the effects that might be produced in the anatomy.
What is Herniated Disc Neuroforaminal Stenosis?
Foraminal stenosis is described as a closing off of the normal spaces through which the spinal nerve roots exit the vertebral column. This is most often the direct result of arthritic osteophyte build up, but can also come about from a herniated disc which presses into the neuroforaminal space. This latter event is often referred to as a foraminal herniated disc.
This process of foraminal narrowing is harmless unto itself, but can cause symptoms if the exiting nerve is compressed. Most intervertebral disc-related foraminal stenosis involves considerable speculation as to whether the herniated disc even touches the suspected nerve structure; forget about positive diagnosis of neurological compression.
Furthermore, if the nerve was truly being compressed, the result would be objective numbness in the areas of the anatomy served. In essence, we are talking about a total lack of nerve signal. In fact, this symptomatic expression is very rare, as most patients report pain, tingling and subjective numbness, which may not necessarily be related to the coincidental bulging spinal disc.
Herniated Disc Foraminal Stenosis Dilemma
It is strange that the very same cause of pain in some patients is the actual cure which is attempted in others. Doctors use various methods of burning, cutting or tying off a nerve to provide relief, since it is well known that a nerve which can not signal, should not be capable of causing pain.
Research clearly shows that a truly compressed nerve can not signal, so how is it possible to create pain? It is a bit illogical in many cases. Of course, some care providers can claim the nerve is only partially compressed, but this theory has also been put to rigid testing. In these cases, the nerve will usually function normally and not produce any atypical signals, such as pain, as long as it still has some freedom to avoid the full mass effect of the disc.
All of this research evidence definitely pokes holes in the structural model that is typically used to diagnose most patients with speculative compressive neuropathy conditions.
Herniated Disc Neuroforaminal Stenosis Tips
We see many pain syndromes which look like symptomatic foraminal stenosis, for sure. Patients demonstrate an intervertebral herniation at a particular level, which has been cited as impinging into the neuroforaminal space. However, upon clinical study of the symptomology, holes appear in the diagnostic theory.
Most patients have symptoms which are far too widespread to account for the impinged nerve root level. Their pain is simply too diversified in location and expression. Additionally, the symptoms are often bilateral, when the stenosis is only on one side. In these cases, it is obvious that the diagnosis is based upon structural defects that might surely be present, but are certainly not responsible for creating the entire symptomatic pattern, if any at all.
Remember also, that unlike arthritic changes leading to foraminal narrowing, many intervertebral disc nerve compression scenarios will resolve completely, all by themselves. It is rare for an acutely prolapsed disc to be able to maintain the pressure against a nerve root over a long period of time.
Instead, the disc will usually lose mass or inflammation, causing it to recede from the foraminal opening and release the nerve. This is further evidence that chronic pinched nerve symptoms might be unrelated to time-resolved disc pathologies.
Herniated Disc > Herniated Disc Facts > Herniated Disc Neuroforaminal Stenosis





