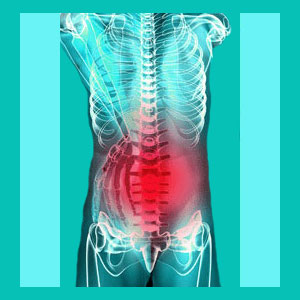
Herniated disc recurrence describes an acute flare-up of pain associated with a bulging or ruptured intervertebral disc pathology. It is extremely common for patients to suffer recurrent painful attacks as part of a herniated disc diagnosis.
What is not always clear is the actual cause of recurrent periods of pain. In many instances, these attacks are blamed on particular life activities, such as too much exercise, bending the wrong way or lifting something heavy. In other circumstances, the pain may be linked to positional complaints, such as standing, sitting or lying down.
This article examines why so many patients experience recurrent herniated disc pain. We will also advise why it may be best to stop obsessing over understanding why the pain occurs, since this may actually be a contributing factor to acute attacks.
Suffering a Herniated Disc Recurrence
Recurrent disc pain is there for a reason. It is not some random process which happens via the luck of the draw. However, despite a great variety of theories as to why a person may suffer a herniated disc flare-up, most affected patients are powerless to stop future recurrences from traumatizing them.
As mentioned in the introduction, patients may suspect a wide range of possible causes or contributors to their painful episodes. In some cases, the theorized exacerbator may be a real explanation for the new symptoms to exist. In others, the suspected factors may actually be coincidental and are only perceived to cause symptomatic escalation. In these latter examples, the patient is likely to be suffering from conditioned responses, in which perceived patterns which exist incidentally to pain are deemed causative.
Of course, in a few patients, the actual source of the herniated disc recurrence is obvious, such as when an acute injury takes place or some major trauma is endured, physically or emotionally.
In a minority of cases, there may be no actual or perceived cause for the escalation of symptoms to occur. In these circumstances, there may be some structural or psychological issues which suddenly worsened, necessitating the present acute expression of agony.
Recurring Herniated Discs
There is really no sure way to truly comprehend why any given patient might suffer a relapse. The possibilities for causative and contributory factors are simply too vast. However, it is safe to say, based on research statistics, that most people with herniated discs do have occasional or even regular flare-ups which temporarily disable them.
Doctors all have their own thoughts on why this occurs, so asking a number of physicians for their opinions will probably result in getting an assortment of speculative answers.
Another interesting statistical fact is that given a significant relapse, many patients fear the worst and undergo new diagnostic testing to see what additional damage must have been caused to their spine. Data suggests that the overwhelming majority will not suffer any worsening of the structural issues suspected of causing their pain, compared to previous imaging studies. Interestingly enough, some people will actually demonstrate a slight to noticeable improvement in these same structural issues, despite the new episode of terrible herniated disc pain.
Herniated Disc Recurrence Experiences
I know what it is like to have recurrent bouts of acute herniated disc pain. I understand how these events typically form a chronic pattern of suffering over many years. I know the frustration of spending all your time, effort and money on tests which offer no concrete explanations and treatments which do nothing to cure you. I understand the same frustration dealing with the lack of a cohesive answer from any doctor as to why the pain will not go away.
For decades, and especially in the first 15 years of my own painful experience, I suffered regular recurrent set backs of acute pain. Fortunately, I was able to end my pain completely and life is much better now.
Can Herniated Discs Come Back?
I can not tell you why your pain has worsened. I doubt that anyone can; at least not definitively. I can tell you that herniated disc recurrences can become patterned events in life and many may not be linked to the typical reasons blamed for them. In fact, many of the contributory reasons may be subtle and not physically-motivated.
In essence, never underestimate the relationship between the presence of life stressors and the occurrence of recurrent flare-ups of pain. These stresses might be conscious and bothering you right now or they may be repressed. In the latter case, the patient is truly defenseless against them, since they have no active knowledge that there is an emotional problem somewhere in the recesses of their mind.
This is not to say that physical factors can not be causative, as well, for they can. However, being that you really can not know for sure what factors are actually damaging, and which may be simply programmed responses, then you must live in fear of everything, which in itself can cause acute attacks of pain.
Talk to your doctor and physical therapist to ascertain all the pieces of the puzzle which may increase the incidence of recurrent pain events. Don’t forget to include your own external observations and internal emotional issues in the mix. However, one of the best ways to prevent recurrences is truly to purge these factors from your mind and carry on with life unaffected. I know it is easy to say and hard to do, but studies suggest it is perhaps the most effective and proactive thing you might accomplish in stopping future flare-ups from taking place.
Herniated Disc > Herniated Disc Advice > Herniated Disc Recurrence





